NBME 16 – Block 4
Quiz Summary
0 of 50 Questions completed
Questions:
Information
You have already completed the quiz before. Hence you can not start it again.
Quiz is loading…
You must sign in or sign up to start the quiz.
You must first complete the following:
Results
Results
0 of 50 Questions answered correctly
Your time:
Time has elapsed
You have reached 0 of 0 point(s), (0)
Earned Point(s): 0 of 0, (0)
0 Essay(s) Pending (Possible Point(s): 0)
Categories
- Not categorized 0%
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- Current
- Review
- Answered
- Correct
- Incorrect
-
Question 1 of 50
1. Question
A 30-year-old man comes to the office for evaluation. He was assigned female at birth and has a vagina. He has a 2-week history of pelvic fullness and increasingly frequent episodes of urinary frequency. He has not had vaginal bleeding. He has no history of serious illness or surgical procedures. His only medication is testosterone. He does not smoke cigarettes, drink alcoholic beverages, or use other substances. Temperature is 37.0°C (98.6°F), pulse is 80/min, respirations are 20/min, and blood pressure is 140/85 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 100%. Pelvic examination shows a firm, mobile, nontender central pelvic mass. Which of the following is the most appropriate next step in diagnosis?
CorrectIncorrect -
Question 2 of 50
2. Question
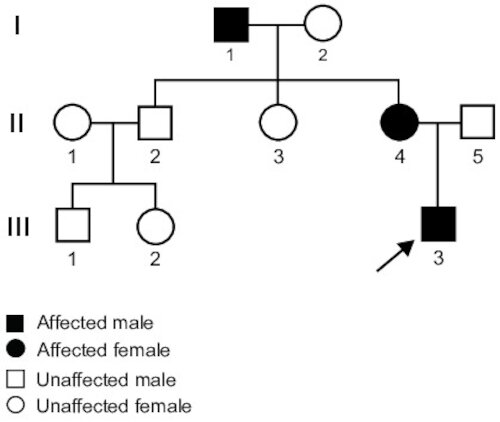
A 2-month-old boy is brought to the physician by his mother for a well-child examination. Physical examination shows melanotic macules on the lips and over the oral mucosa. Several other family members have similar symptoms and rectal bleeding. A pedigree is shown; the patient is III-3. This patient should be monitored for which of the following?
CorrectIncorrect -
Question 3 of 50
3. Question
A 5-year-old boy is brought to the physician by his mother for removal of a tick from his right arm. She says he was playing outside with his dog this morning; she noticed the tick when he came inside for lunch. He has no history of serious illness and receives no medications. Vital signs are within normal limits. Examination shows a small, nonengorged deer tick attached to the skin over the right upper extremity. There is no rash. The remainder of the examination shows no abnormalities. In addition to removal of the tick, which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 4 of 50
4. Question
A 56-year-old woman comes to the office because of a 3-month history of vaginal pain during sexual intercourse with her husband. She also has post-void dribbling that requires the use of absorbent pads, and she occasionally has the urge to urinate without warning. She has had three urinary tract infections treated with antibiotics during the past 4 months. Last menses occurred 2 years ago. She has no history of serious illness and takes no other medications. Vital signs are within normal limits. Pelvic examination shows an anterior vaginal wall mass; palpation of the mass produces pain. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 5 of 50
5. Question
A 46-year-old woman comes to the emergency department 1 hour after she had a 15-minute episode of chest pain during a routine examination at her primary care physician’s office. ECG performed during the episode showed 4 mm of ST-segment elevation in leads II, III, and aVF. She has a 6-month history of intermittent, mild substernal chest pain. The episodes occur twice monthly, usually while at rest and during the night, and last 15 minutes before resolving spontaneously. Exercise stress test and coronary angiography performed during the past year showed no abnormalities. She also has migraines and intermittent heartburn. She has no history of diabetes mellitus, hypertension, or hyperlipidemia. Medications are omeprazole and ibuprofen. There is no family history of premature coronary artery disease. The patient has smoked one pack of cigarettes daily for 25 years. Vital signs are within normal limits. Cardiac examination shows no abnormalities. Serum troponin I concentration is within the reference range. ECG shows no abnormalities. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 6 of 50
6. Question
A 35-year-old woman, gravida 1, para 1, comes to the office for a health maintenance examination. Ten years ago, she had uncomplicated spontaneous vaginal delivery of healthy female newborn, whom she breast-fed for 15 months. The patient’s vaccinations are up-to-date. Family history is remarkable for postmenopausal breast cancer in her maternal aunt, heart disease in her paternal grandfather, and stroke in her maternal grandmother. The patient’s mother has hypertension, and her father was recently diagnosed with coronary artery disease. The patient drinks two glasses of wine once monthly. She does not smoke cigarettes or use other substances. She is sexually active with a new male partner. She exercises regularly. Vital signs are within normal limits. Physical examination discloses no abnormalities; specimen for cervical cancer screening is collected today. After providing her with information about how to obtain the cervical cancer screening results, which of the following is the most appropriate screening recommendation for this patient?
CorrectIncorrect -
Question 7 of 50
7. Question
A 25-year-old man comes to the office because of a 1-month history of shortness of breath; he has had a 6.8-kg (15-lb) weight loss during this period. Respirations are 22/min. A 1-cm, raised, irregular lesion is noted on the upper back. The lesion is black with gray areas. The remainder of the examination discloses no abnormalities. The physician suspects metastatic disease. A chest x-ray is most likely to show which of the following bilaterally in this patient?
CorrectIncorrect -
Question 8 of 50
8. Question
A 14-year-old boy is brought to the ambulatory surgical center by his parents for elective surgical repair of an anterior cruciate ligament injury. Medical history is remarkable for reactive airway disease. His only medication is albuterol as needed. After his parents leave the examination room, the patient informs the physician that he uses electronic cigarettes containing nicotine and marijuana daily. The patient is at the 50th percentile for height and weight; BMI is at the 48th percentile. Vital signs are within normal limits. Physical examination discloses no unexpected abnormalities. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 9 of 50
9. Question

A 6-week-old male infant is brought to the office by his mother 5 days after she noticed a spot on his cheek that is increasing in size. The spot was not present at the patient’s last well-child examination 2 weeks ago. He was born at term following an uncomplicated pregnancy and spontaneous vaginal delivery. Apgar scores were 9 and 10 at 1 and 5 minutes, respectively. Growth and development are appropriate for age. He is exclusively breast-fed. A photograph of the lesion is shown. The lesion is easily compressed and is not ulcerated. No other abnormalities are noted. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 10 of 50
10. Question
The physician in charge at a skilled nursing care facility instructs a nurse to administer intramuscular influenza vaccine to specific older residents. The vaccine comes in multiple-dose vials that are capped with a rubber stopper. In describing the protocol, the physician tells the nurse to obtain consent, check for allergies, and swab the rubber stopper of the vial and each skin injection site with alcohol before administering the vaccine. Which of the following additional aseptic procedures is most appropriate in this situation?
CorrectIncorrect -
Question 11 of 50
11. Question
Patient Information
Age: 78 years
Gender: M, self-identified
Race/Ethnicity: Native American, self-identified
Site of Care: hospital
History
Reason for Admission/Chief Concern: day 4 of hospitalization following aortobifemoral bypass grafting
History of Present Illness:
• 10-year history of aortoiliac occlusive disease
• received antibiotic therapy prior to aortobifemoral bypass grafting
• received heparin and 2 units of packed red blood cells intraoperatively
• uncomplicated postoperative course
• scheduled for discharge tomorrow to rehabilitation facility
• now reports 3-hour history of pain and discoloration in right great toe
Additional Past Medical History:
• chronic obstructive pulmonary disease
• type 2 diabetes mellitus
• hypertension
• gout
• coronary artery disease
• coronary artery bypass grafting 3 years ago
• right hip fracture and replacement 2 years ago; developed postoperative deep venous thrombosis treated with heparin and 3 months of warfarin
Medications:
• aspirin
home, continued on admission
• atorvastatin
home, continued on admission
• metformin
home, continued on admission
• lisinopril
home, continued on admission
• albuterol inhaler prn for dyspnea
home, continued on admission
• heparin
initiated intraoperatively, continued postoperatively
• oxycodone
initiated postoperatively
• allopurinol
home, temporarily discontinued on admission
Allergies:
• no known drug allergies
Psychosocial History:
• smoked one pack of cigarettes daily for 60 years
• does not drink alcoholic beverages or use other substances
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
37.1°C
64/min
16/min
138/86 mm Hg
98%
174 cm
80 kg
26 kg/m2
(98.8°F)
on 1L NC
(5 ft 9 in)
(176 lb)
• Appearance: alert; minimal distress
• Skin: incisions clean, dry, and intact with staples; ecchymosis over trunk and all extremities
• Pulmonary: clear to auscultation; expiratory wheezes
• Cardiac: regular rhythm; no murmurs, rubs, or gallops
• Abdominal: nondistended; soft, nontender to palpation
• Extremities: Doppler ultrasonography discloses strong signals in left posterior tibial artery and dorsalis pedis artery and weak signals in right posterior tibial artery and dorsalis pedis artery; bluish coloration of right great toe; toe is tender to palpation
• Neurologic: fully oriented
Diagnostic Studies
Serum
Na+
139 mEq/L
K+
4.2 mEq/L
Cl–
100 mEq/L
HCO3–
24 mEq/L
Urea nitrogen
15 mg/dL
Creatinine
1.2 mg/dL
Glucose, nonfasting
192 mg/dL
Blood
Hematocrit
36%
Hemoglobin
12.2 g/dL
WBC
7500/mm3
Platelet count
35,000/mm3
Question: Which of the following is the most appropriate next step in pharmacotherapy?
Option
Discontinue
Initiate
A
Heparin
Argatroban
B
Heparin
Enoxaparin
C
Heparin
Warfarin
D
Oxycodone
Allopurinol
E
Oxycodone
Gabapentin
F
Oxycodone
Morphine
CorrectIncorrect -
Question 12 of 50
12. Question
A 9-month-old boy is brought to the physician for a well-child examination. His mother reports that he has had a slightly decreased appetite and activity level during the past month but has been otherwise well. His temperature is 37.5°C (99.5°F), pulse is 155/min, and blood pressure is 109/60 mm Hg. Examination shows a firm, irregular, nontender mass in the right side of the abdomen. An abdominal CT scan shows an 8-cm retroperitoneal mass displacing the right kidney inferiorly. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 13 of 50
13. Question
A 41-year-old man comes to the office for a follow-up examination. He has schizophrenia, and his symptoms have been well managed since he began taking haloperidol 2 years ago. Recently, auditory hallucinations have been mild; he hears “an occasional whisper,” but it does not cause distress. He “self-medicated” with cocaine in the past but has not used it during the past 2 years. He recently married. He plans to complete a masters program in computer science this year. Vital signs are within normal limits. Physical examination discloses no abnormalities. On mental status examination, he has a euthymic mood and congruent affect. Thoughts are linear and well organized. Which of the following studies is most appropriate to obtain periodically to monitor this patient’s long-term care?
CorrectIncorrect -
Question 14 of 50
14. Question
A 3-year-old boy is brought to the physician because his mother is concerned about his short stature. He has reached all developmental milestones. She reports that the patient’s 7-year-old brother was at the 40th percentile for height at this age. The older brother wears a hearing aid. On examination, the patient is at the 3rd percentile for height and weight. The remainder of the examination shows no abnormalities. Laboratory studies show:
Serum
Na+
138 mEq/L
K+
2.8 mEq/L
Cl−
112 mEq/L
HCO3−
16 mEq/L
Ca2+
9.2 mg/dL
Urea nitrogen
6 mg/dL
Glucose
98 mg/dL
Creatinine
0.4 mg/dL
Phosphorus
2.6 mg/dL
Uric acid
6.1 mg/dL
Urine
pH
7.2
Specific gravity
1.012
Protein
none
Glucose
none
RBC
0/hpf
WBC
0/hpf
Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 15 of 50
15. Question
A 32-year-old woman is admitted to the intensive care unit after she was involved in a motor vehicle collision. She was intubated and mechanically ventilated at the scene by emergency services personnel when they determined that she was not breathing. CT scan of the head shows a large subdural hematoma and two areas of intracerebral bleeding. The subdural hematoma is evacuated. On postoperative day 2, the patient remains comatose and ventilator dependent. Blood pressure is 110/60 mm Hg. There are no spontaneous respirations. The surgical site is clean and intact. On neurologic examination, the pupils are fixed at the midposition and not reactive to light; there are no corneal reflexes. Doll’s eye (oculocephalic) reflex is absent. There is no gag reflex with suctioning. The patient does not respond to painful stimuli. The remainder of the examination discloses no abnormalities. Which of the following is the most appropriate next step when considering whether to withdraw life support from this patient?
CorrectIncorrect -
Question 16 of 50
16. Question
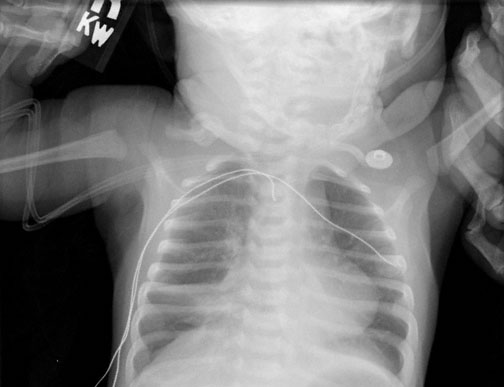
A 2-month-old boy is brought to the emergency department by his parents 30 minutes after he stopped breathing and turned blue while the parents were laying him down for a nap. They say he resumed breathing after 25 seconds when they rubbed his chest. He has a 1-day history of cough, nasal congestion, and decreased feeding and activity. He has not had fever. He has no history of serious illness and receives no medications. Vaccinations are up-to-date. Temperature is 37.9°C (100.3°F), pulse is 140/min, respirations are 65/min, and blood pressure is 100/70 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 90%. Examination shows nasal congestion and rhinorrhea. Diffuse wheezes are heard bilaterally, and there are subcostal retractions. The remainder of the examination discloses no abnormalities. Chest x-ray is shown. Which of the following is most likely to confirm the etiology of this patient’s episode?
CorrectIncorrect -
Question 17 of 50
17. Question
A 46-year-old woman comes to the clinic because of a 6-month history of poor sleep and night sweats. Previously her sleep pattern was normal. She falls asleep easily but frequently wakes perspiring and feeling overheated. The night sweats typically occur several times nightly, and happen most frequently after drinking two glasses of red wine before bed, which she does 3 to 4 nights weekly. The patient reports no changes in appetite or mood. She has no history of serious illness, and her only medication is a multivitamin. Menses occur at regular 30- to 32-day intervals. She does not smoke cigarettes or use any other substances. She is sexually active with one female partner and has no pain with intercourse. The patient drinks three cups of coffee daily and exercises for 30 minutes daily. She is 162 cm (5 ft 4 in) tall and weighs 61 kg (134 lb); BMI is 23 kg/m2. Vital signs are within normal limits. She appears fatigued. Physical examination discloses no abnormalities. Results of complete blood count and serum TSH concentration are within the reference ranges. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 18 of 50
18. Question
Patient Information
Age: 6 years
Sex Assigned at Birth: F
Race/Ethnicity: unspecified
Site of Care: clinic
History
Reason for Visit/Chief Concern: “My daughter has had trouble hearing for the past 24 hours.”
History of Present Illness:
• decreased hearing in left ear
• slight itching and pain “inside the ear hole”
• pain rated as 3/10
• no drainage noted
• has not inserted anything into the ear
Past Medical History:
• mild, intermittent asthma
• no history of ear infections
Medications:
• albuterol prn for wheezing
Vaccinations:
• up-to-date
Allergies:
• no known drug allergies
Family History:
• mother and father: alive with no chronic conditions or hearing difficulties
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
37.0°C
88/min
22/min
92/56 mm Hg
100%
115 cm
20 kg
15 kg/m2
(98.6°F)
on RA
(3 ft 9 in)
(44 lb)
47th %ile
50th %ile
50th %ile
• Appearance: alert, cooperative
• Skin: no rash
• HEENT: moist mucous membranes; left ear has white discharge in the canal with an erythematous tympanic membrane and canal; left tympanic membrane mobile with insufflation, no fluid level; pain on traction of pinna; no mastoid tenderness; right ear shows no abnormalities
• Neck: supple; no cervical lymphadenopathy
Question: Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 19 of 50
19. Question
A 76-year-old man comes to the emergency department because of a 1-day history of severe right-sided facial pain and swelling, fever, and difficulty swallowing. Two weeks ago, he underwent uncomplicated laparoscopic cholecystectomy. He has hypertension treated with hydrochlorothiazide. He does not smoke cigarettes or use illicit drugs. He drinks two glasses of wine daily. He has been in a monogamous relationship with his male partner for 40 years. The patient’s temperature is 39.3°C (102.7°F), pulse is 92/min, respirations are 20/min, and blood pressure is 110/54 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 99%. Examination shows erythema and severe tenderness to palpation of the right pre- and postauricular areas extending to the mandible. Purulent material is expressed from the parotid duct. The lymph nodes in the submandibular region are small and tender to palpation. The abdominal incision is clean and dry. The remainder of the examination shows no abnormalities. Which of the following is the most likely causal agent?
CorrectIncorrect -
Question 20 of 50
20. Question
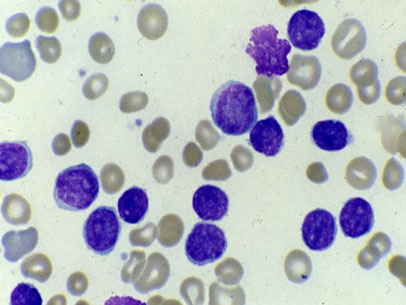
A 6-year-old girl is brought to the office because of a 2-week history of diffuse aches in her arms, legs, and back and decreased energy. She has not had changes in appetite during this period. She has no history of serious illness. She is at the 10th percentile for height and weight. Vital signs are within normal limits. The patient appears pale but is not in acute distress. Examination shows no rash or petechiae. Shotty lymph nodes are palpated over the cervical and axillary areas. Cardiopulmonary examination shows no abnormalities. The abdomen is soft; there is no organomegaly. There is diffuse, nonspecific tenderness to palpation over the bones of the upper and lower extremities and back. Examination of the joints shows no swelling, erythema, or warmth. Hemoglobin concentration is 9.4 g/dL (N=11.5–14.5), leukocyte count is 5600/mm3, and platelet count is 106,000/mm3. X-rays of the long bones show osteolytic lesions. Blood smear is shown. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 21 of 50
21. Question
Patient Information
Age: 70 years
Gender: M, self-identified
Race/Ethnicity: unspecified
Site of Care: office
History
Reason for Visit/Chief Concern: “I have dizzy spells”
History of Present Illness:
• 3-month history of progressively frequent episodes of dizziness
• episodes occur when patient gets out of bed in the morning and when he stands up quickly from seated position
• episodes last from approximately 30 seconds to between 2 and 5 minutes
• dizziness subsides with sitting or resting
• no fever, chills, or chest pain
• no syncope
• has been adherent to current medication regimen
Past Medical History:
• type 2 diabetes mellitus; home blood glucose monitoring once daily shows glucose concentrations ranging from 180 to 200 mg/dL
• hypertension
• major depressive disorder
Medications:
• glipizide
• metformin
• hydrochlorothiazide
• sertraline
Allergies:
• ACE inhibitors (cough)
Psychosocial History:
• drinks two alcoholic beverages two to three times weekly
• does not smoke cigarettes
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
37.0°C
75/min supine
14/min
135/84 mm Hg supine
97%
180 cm
85 kg
26 kg/m2
(98.6°F)
80/min standing
105/65 mm Hg standing
on RA
(5 ft 11 in)
(187 lb)
• Appearance: well; no acute distress
• Skin: no rashes or lesions
• HEENT: PERRL; ocular movements full; moist oral mucosa
• Pulmonary: clear to auscultation; symmetric chest expansion
• Cardiac: regular rhythm; no murmurs, rubs, or gallops
• Abdominal: soft; nondistended; nontender to palpation
• Extremities: no edema
• Neurologic: decreased sensation to pinprick in stocking distribution over feet
Diagnostic Studies
Serum
Na+
140 mEq/L
K+
4.0 mEq/L
Cl–
100 mEq/L
HCO3–
24 mEq/L
Urea nitrogen
14 mg/dL
Creatinine
0.8 mg/dL
Glucose, nonfasting
180 mg/dL
Blood
Hematocrit
42%
Hemoglobin
14.0 g/dL
WBC
6000/mm3
Neutrophils, segmented
62%
Neutrophils, bands
3%
Lymphocytes
33%
Monocytes
2%
Platelet count
250,000/mm3
Hemoglobin A1c
9.0%
Question: Which of the following is the most likely underlying cause of this patient’s condition?
CorrectIncorrect -
Question 22 of 50
22. Question
A prospective study is conducted to assess the effectiveness of tamoxifen as an adjuvant therapy for premenopausal patients with stage I breast cancer who have undergone lumpectomy. A total of 1000 patients from hospitals around the USA are enrolled. The results of this study are compared with those of a previous study of 400 patients with stage I breast cancer treated with lumpectomy who did not receive tamoxifen. Results of the current study show reduced local recurrence of breast cancer in patients treated with tamoxifen. Which of the following raises the most concern about this study?
CorrectIncorrect -
Question 23 of 50
23. Question
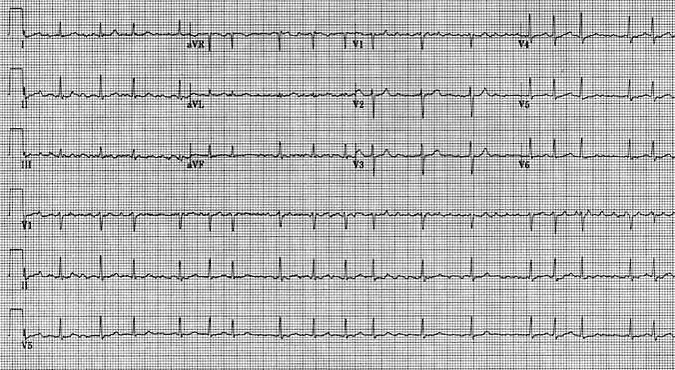
A 59-year-old man is brought to the emergency department 40 minutes after the sudden onset of left-sided weakness. The weakness has not changed in severity during this time. He has a 5-year history of hypertension and a 10-year history of hypercholesterolemia. His medications are lisinopril and atorvastatin. Pulse is 82/min and irregular, respirations are 12/min, and blood pressure is 142/84 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 96%. On examination, a grade 2/6, right carotid bruit is heard. There is severe weakness of the lower left side of the face. Muscle strength is 3/5 in the left upper extremity and 3/5 in the proximal aspect of the left lower extremity. Muscle tone is decreased and deep tendon reflexes are 1+ in the left upper extremity. Sensation to light touch is severely decreased over the left side of the face, left upper extremity, and left side of the trunk. Proprioception is absent in the left upper extremity. Finger-stick blood glucose concentration is 138 mg/dL. ECG is shown. CT scan of the head without contrast shows no abnormalities. Which of the following is the most appropriate next step in management of this patient’s weakness?
CorrectIncorrect -
Question 24 of 50
24. Question
A 21-year-old woman, gravida 2, para 2, comes to the office because of moderate pain, redness, and swelling of her left nipple while breast-feeding. She delivered a healthy male newborn 2 weeks ago. Application of hot compresses and ibuprofen have not provided relief. She has no history of serious illness. Her only other medication is a prenatal vitamin. Temperature is 37.3°C (99.1°F), pulse is 72/min, respirations are 12/min, and blood pressure is 95/55 mm Hg. Examination of the left breast shows an area of tenderness, induration, and erythema around the nipple; there is no nipple retraction or underlying fluctuance. Which of the following is the most appropriate next step in diagnosis?
CorrectIncorrect -
Question 25 of 50
25. Question
A clinician would like to evaluate the efficacy of a new asthma medication for preventing asthma exacerbations requiring hospitalization among adult patients. Two hundred patients, aged 18 to 65 years with asthma diagnosed via spirometry, are enrolled from general internal medicine clinics. The patients are randomized to receive either the new medication plus standard therapy or placebo plus standard therapy. Patients are observed for 2 years and undergo spirometry every 6 months. At the end of the study, FEV1 increased by 14% from baseline in patients who received the new medication and decreased by 2% from baseline in patients who received placebo (P=.01). The clinician concludes that the new medication decreases the risk for hospitalization in adults with asthma. Which of the following most limits confidence in the clinician’s conclusion?
CorrectIncorrect -
Question 26 of 50
26. Question
A 5-month-old girl is brought to the office by her parents to establish care. Her parents are concerned that she seems less active than their friend’s infant of the same age. The parents say she does not try to roll over and seems content just lying down for long periods of time. They report that she is interactive, smiles and coos, and is a “very happy baby.” The infant was born at 38 weeks’ gestation to a 28-year-old primigravid woman via uncomplicated spontaneous vaginal delivery at home. Her parents declined routine perinatal medical care. Medical history is unremarkable and she receives no medications. The infant is breast-feeding well and the parents have started introducing solid foods to her diet. She sleeps through the night and takes two naps daily. Family history is unremarkable. She is 65.5 cm (25.8 in; 75th percentile) long and weighs 7.4 kg (16.3 lb; 75th percentile); head circumference is 42.4 cm (16.7 in; 75th percentile). Vital signs are within normal limits. The infant is smiling and interactive. Physical examination shows a tremor of the tongue. When held upright, she seems to slip through the physician’s hands and when held in a prone position, she does not hold her head up. She holds a plastic toy but does not bring it to her mouth. The remainder of the physical examination discloses no abnormalities. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 27 of 50
27. Question
A previously healthy 50-year-old man comes to the physician because of a 2-month history of abdominal pain that is more severe after eating. His uncle died of gastric cancer at the age of 40 years. His vital signs are within normal limits. Physical examination shows epigastric tenderness. Laboratory studies show a hemoglobin concentration of 11 g/dL, hematocrit of 33%, and mean corpuscular volume of 70 μm3. Test of the stool for occult blood is positive. An upper endoscopy shows a gastric ulcer. An ulcer biopsy specimen is positive for urease. In addition to amoxicillin and omeprazole, which of the following is the most appropriate pharmacotherapy?
CorrectIncorrect -
Question 28 of 50
28. Question
A 3-month-old boy is brought to the clinic by his parents because of a 1-week history of rash. His mother initially noticed the rash on his face, but it has now spread to both arms. He has not had fever, vomiting, or diarrhea. Medical history is unremarkable and he receives no medications. He was born at 37 weeks’ gestation to a 23-year-old woman, gravida 2, para 1, via uncomplicated repeat caesarean delivery. At birth he was 49.5 cm (19.5 in; 40th percentile) long and weighed 3200 g (7 lb 1 oz; 35th percentile); head circumference was 34.3 cm (13.5 in; 40th percentile). Vaccinations are up-to-date. He has no known drug allergies. He lives at home with his parents and 3-year-old sister. Today he is 60.4 cm (23.8 in; 30th percentile) long and weighs 5.7 kg (12.5 lb; 40th percentile); head circumference is 40.6 cm (16 in; 45th percentile). Rectal temperature is 37.5°C (99.5°F), pulse is 140/min, respirations are 24/min, and blood pressure is 85/50 mm Hg. Skin examination shows erythematous papules and vesicles with some scaling on the face and the extensor surfaces of both upper extremities. There are petechiae on the trunk and all four extremities and two small bruises on the lower extremities. The remainder of the physical examination discloses no abnormalities. Results of laboratory studies are shown:
Blood
Hematocrit
37% (N=32%–42%)
Hemoglobin
13.1 g/dL (N=10.5–14)
WBC
7200/mm3 (N=6000–14,000)
Neutrophils, segmented
59%
Lymphocytes
32%
Monocytes
7%
Eosinophils
2%
Platelet count
30,000/mm3
Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 29 of 50
29. Question
A 62-year-old man comes to the office because of a 2-week history of intermittent temperatures to 37.9°C (100.2°F) and fatigue. He otherwise feels well. Medical history is remarkable for hypertension, hyperlipidemia, and benign prostatic hyperplasia. Medications are lisinopril, atorvastatin, and 81-mg aspirin. He does not smoke cigarettes, drink alcohol, or use other substances. Temperature is 37.6°C (99.7°F), pulse is 62/min, respirations are 14/min, and blood pressure is 130/80 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 97%. Lungs are clear to auscultation. Cardiac examination discloses a grade 2/6, systolic, crescendo-decrescendo murmur that is heard best at the upper right sternal border and radiates to the neck; a grade 2/6 holosystolic murmur is heard best at the apex and radiates to the axilla. The remainder of the examination shows no abnormalities. Results of laboratory studies are shown:
Hemoglobin
11.2 g/dL
Hematocrit
34%
Leukocyte count
7000/mm3
Platelet count
300,000/mm3
Two blood cultures grow Streptococcus bovis. Transthoracic echocardiography shows a mobile vegetation on the mitral valve. In addition to beginning antibiotic therapy, which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 30 of 50
30. Question
A 33-year-old woman returns to the office for follow-up of chronic malnutrition secondary to Crohn disease. At her last visit 6 months ago, she reported diarrhea and weight loss of 5 pounds. Loperamide was recommended at that time. Today, she reports continued diarrhea after meals and fatigue. Surgical history is remarkable for ileocecectomy 10 years ago for management of Crohn disease and exploratory laparotomy 10 months ago for management of a small bowel obstruction. During the most recent procedure, the patient underwent extensive lysis of adhesions and resection of 10 cm of her small bowel. During the past 2 weeks, she has developed green drainage from her midline incision that is worse after meals. Additional medications are infliximab and prednisone. She is 160 cm (5 ft 3 in) tall and weighs 47.5 kg (105 lb); BMI is 19 kg/m2. Temperature is 37.3°C (99.2°F), pulse is 101/min, respirations are 18/min, and blood pressure is 102/76 mm Hg. Abdominal examination shows a midline incision with a 0.5-cm area at the lower aspect that is open. A bandage that was removed from the open area prior to examination is stained with bilious drainage. Which of the following factors in this patient’s history is the strongest indication for total parenteral nutrition?
CorrectIncorrect -
Question 31 of 50
31. Question
A 6-year-old boy is brought to the office by his adoptive parents because of an 18-month history of disruptive behaviors. The patient had been placed with his current family 18 months ago and was adopted 6 months ago. The patient was removed from the care of his biological parents because of neglect with subsequent termination of parental rights. Since placement with his current adoptive parents, the patient has often appeared irritable and sad every day. His parents say he often screams, rarely smiles, and pushes them away when they attempt to comfort him. They say, “We were hoping that he would change his behavior after the adoption, but that has not happened.” He sometimes is able to interact appropriately with his parents and peers but often withdraws into himself. Medical history is unremarkable and he receives no medications. The patient is at the 25th percentile for height and 15th percentile for weight; BMI is at the 17th percentile. Vital signs are within normal limits. During the examination, the patient sits alone in the corner, stares at the physician with a blank expression, has limited spontaneous movements, and refuses to answer questions. Physical examination discloses no abnormalities. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 32 of 50
32. Question
A 42-year-old woman, gravida 3, para 2, at 10 weeks’ gestation comes to the office for her first prenatal visit. Previous pregnancies were uncomplicated and ended in uncomplicated spontaneous vaginal deliveries at term. She has no history of serious illness, and her only medication is a prenatal vitamin. Vital signs are within normal limits. Examination shows a uterus consistent in size with a 10-week gestation. The patient says she is worried about the risk for fetal genetic abnormalities because of her advanced age. She wishes to pursue as soon as possible a genetic screening test that would have a high likelihood of detecting Down syndrome. Which of the following is the most appropriate screening test for this patient?
CorrectIncorrect -
Question 33 of 50
33. Question
A 21-year-old man comes to the office for a routine examination. He is due for the tetanus toxoid, diphtheria toxoid, and acellular pertussis (Tdap) vaccine. The physician orders the vaccine, and one of the nurses administers it. After the patient leaves, it is noted that the patient received the tetanus and diphtheria toxoid (Td) vaccine instead. A root cause analysis performed by the clinic team determines that the vials for the two vaccines have similar-colored caps, which contributed to the error. Which of the following is most likely to decrease the likelihood of recurrence of this error?
CorrectIncorrect -
Question 34 of 50
34. Question
A 67-year-old woman comes to the physician because of a 1-year history of moderate shortness of breath with minimal exertion. She becomes short of breath when she does laundry and cannot go shopping without her husband’s assistance. During the past 5 months, she has had several colds and a chronic nonproductive cough. She is worried she might have pneumonia. She takes no medications. She does not smoke. She worked in a bakery for 25 years. Her temperature is 37°C (98.6°F), pulse is 82/min, respirations are 18/min, and blood pressure is 130/84 mm Hg. Crackles are heard over the lower third of the lung fields bilaterally. Pulmonary function tests show a decreased diffusion capacity. An x-ray of the chest shows increased interstitial markings and a normal cardiac silhouette. Which of the following is the most likely underlying mechanism?
CorrectIncorrect -
Question 35 of 50
35. Question
A 42-year-old man comes to the emergency department because of a 1-month history of progressive chronic diarrhea, abdominal bloating, nausea, vomiting, muscle weakness, and palpitations. He also has had an unintentional 6-kg (13-lb) weight loss during this period. He now has 9 to 10 watery bowel movements daily. There is no blood, fat, or mucus in the stool. Fasting and over-the-counter loperamide therapy have not resolved his symptoms. He has not traveled to the tropics recently. He appears ill and lethargic. Temperature is 37.0°C (98.6°F), pulse is 121/min, respirations are 23/min, and blood pressure is 84/55 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 95%. Physical examination shows dry skin with decreased turgor and delayed capillary refill time. Results of serum studies are shown:
Na+
130 mEq/L
K+
2.6 mEq/L
HCO3–
17 mEq/L
Ca2+
11.0 mg/dL
Urea nitrogen
45 mg/dL
Creatinine
1.4 mg/dL
Glucose
172 mg/dL
CT scan of the abdomen and pelvis shows a 4.7-cm, well-defined, partially cystic mass in the tail of the pancreas and a single 6.8-cm partially cystic mass in the left lobe of the liver. An increased serum concentration of which of the following is most likely to confirm the suspected diagnosis in this patient?
CorrectIncorrect -
Question 36 of 50
36. Question
A 53-year-old man comes to the physician because of right heel pain for 3 weeks. He has had similar episodes during the past 2 years that resolved without treatment. He participates in marathons and usually runs 6 miles daily. He has been unable to run lately because of the pain. Physical examination shows tenderness and swelling of the right Achilles tendon. The patient asks the physician if there is anything he can do to prevent future recurrences of the pain. It is most appropriate for the physician to recommend which of the following?
CorrectIncorrect -
Question 37 of 50
37. Question
An 8-week-old boy is brought to the office by his parents because of a 4-day history of increased vomiting after feeding. His mother describes the vomit as white in appearance and says the infant is still hungry and eager to feed after vomiting. He is exclusively bottle-fed with formula. The infant was delivered via spontaneous vaginal delivery at 38 weeks’ gestation. Pregnancy and delivery were unremarkable. Length is 55 cm (21.7 in; 5th percentile), weight is 4.9 kg (10.8 lb; 27th percentile), and head circumference is 39 cm (15.4 in; 53rd percentile). Temperature is 37.0°C (98.6°F), pulse is 170/min, respirations are 50/min, and blood pressure is 80/50 mm Hg. The patient appears lethargic. Physical examination discloses an abdominal mass that is intermittently palpable in the right upper quadrant and wavelike peristaltic contractions. Results of laboratory studies are shown:
Serum
Na+
129 mEq/L
K+
2.7 mEq/L
Cl–
72 mEq/L
HCO3–
37 mEq/L
Urea nitrogen
24 mg/dL
Creatinine
0.5 mg/dL (N=0.03–0.5)
Blood
Hematocrit
41.4% (N=32%–42%)
Hemoglobin
14 g/dL (N=10.5–14)
WBC
12,400/mm3 (N=6000–14,000)
Platelet count
685,000/mm3
Which of the following is the most appropriate next step in evaluation?
CorrectIncorrect -
Question 38 of 50
38. Question
A cardiothoracic surgeon has performed a variety of operations using electrosurgical units during the past 22 years without causing an intraoperative burn. Two weeks ago, his community hospital began using a new model of electrocautery machine. Volume on this machine is controlled by a spin dial. Since that time, two different patients have experienced intraoperative burns. A root cause analysis is conducted and shows that the volume dial on the machine was unintentionally manipulated by the surgical team during the course of surgery. Therefore, the surgical team did not hear the electrocautery machine firing when it was left on the surgical field for too long. Based on these findings, which of the following is the most appropriate immediate action for this hospital to take?
CorrectIncorrect -
Question 39 of 50
39. Question
A 24-year-old man comes to the office for a follow-up examination. Four months ago, he was evaluated because of a painful left deep thigh mass that was noticed 2 weeks after he hit a tree while skiing. At the time of injury, he did not sustain any fractures but had numerous bruises over his chest, left upper extremity, and upper part of the left lower extremity, all of which have resolved. Examination at that time showed a 6-cm mass in the deep muscles of the lateral left thigh. X-ray of the left thigh showed soft tissue swelling but no fracture. He has no personal or family history of major medical illness and takes no medications. Today, vital signs are within normal limits. Examination shows mild decrease in size of the mass to 5 cm in the deep muscles of the left lateral thigh. X-ray of the left thigh shows a rounded mass with smooth peripheral calcification. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 40 of 50
40. Question
A 32-year-old woman comes to the physician because of generalized swelling for 2 weeks. During the past year, she also has had progressive shortness of breath with extreme exertion. She has a 2-year history of frequent colds and bronchitis. She is comfortable at rest. Examination shows jugular venous distention to 10 cm above the sternal angle when the patient is sitting at a 45-degree angle. The lungs are clear to auscultation. Cardiac examination shows an increased S1 and a fixed, wide, split S2 with increased P2. A grade 2/6, systolic ejection murmur is heard best in the pulmonic area. There is moderate clubbing and cyanosis of the extremities. Which of the following is the most likely location of this patient’s primary lesion?
CorrectIncorrect -
Question 41 of 50
41. Question
A 12-year-old girl is brought to the clinic by her cousin after telling the cousin that she tried to complete suicide last night by swallowing a handful of ibuprofen tablets. The patient says she has had mild dizziness and abdominal pain since she woke up this morning. She was diagnosed with major depressive disorder 2 months ago. Her only prescribed medication is sertraline, which has mildly improved her symptoms. Today she reveals that she was sexually abused by a family member 2 years ago but had not felt able to mention it until today; she says she cannot stop thinking about the abuse. She is tearful. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 42 of 50
42. Question
Patient Information
Age: 5 years
Sex: M
Race/Ethnicity: unspecified
Site of Care: emergency department (ED)
History
Reason for Visit/Chief Concern: unrestrained backseat passenger in motor vehicle collision
History of Present Illness:
• car was stopped at a traffic light when it was hit from the rear by a car driving 40 miles per hour
• was found moaning in the back seat by emergency personnel
• was placed in spinal immobilization and a cervical collar was applied at the scene
• 100% oxygen via nonrebreather mask administered en route to the ED
• patient’s mother was the driver and was transported unconscious to another hospital
Past Medical History:
• unknown
Medications:
• unknown
Vaccinations:
• unknown
Allergies:
• unknown
Psychosocial History:
• unknown
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
36.8°C
124/min
32/min
102/70 mm Hg
91%
—
—
—
(98.2°F)
on 100% O2 via NRB face mask
• Appearance: unresponsive; lying on spine board; cervical collar in place
• Skin: pale and mottled
• HEENT: PERRL; no trauma to face noted; oropharynx without
lesions; nares patent
• Pulmonary: bilateral breath sounds heard on auscultation
• Cardiac: no murmurs, rubs, or gallops
• Abdominal: soft; no masses
• Extremities: deformation of the left forearm with good distal pulse
• Neurologic: unresponsive to painful stimuli in upper and lower extremities
Question: Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 43 of 50
43. Question
Physician A is approached by Physician B at the hospital 18 hours after Physician B “threw out” his low back. Physician B is on service, and he says that none of his partners are available to cover for him. He cannot get an appointment with his physician for 3 days. He appears desperate, agitated, and in distress; his pager is buzzing repeatedly. He is walking stiffly and seems to be in severe pain every time he moves. He asks, “Could I impose on you to write me a prescription for 60 oxycodone tablets to help me until I can see my physician?” Physician A denies this request, saying he has a policy against prescribing controlled substances outside of the office. Later that afternoon, Physician A runs into one of his physician partners, who confides that the Physician B had asked him yesterday for 60 oxycodone tablets. The two physician partners are concerned that Physician B may have a drug problem. Which of the following is the most appropriate next step by the physician partners?
CorrectIncorrect -
Question 44 of 50
44. Question
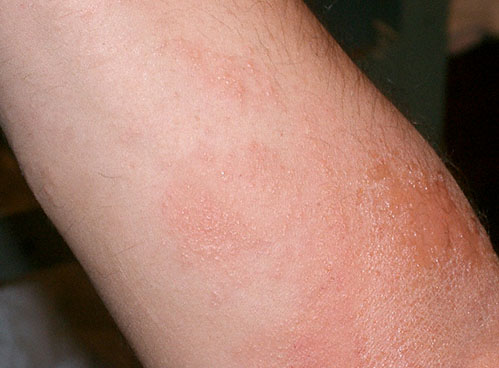
A 37-year-old woman comes to the clinic because of a 4-day history of severe redness, itchiness, and streaks of blistering over her forearms and hands. She has had no other symptoms. Medical history is unremarkable. Medications are an oral contraceptive and as-needed ibuprofen. The patient lives in a heavily wooded area and says she has been gardening during the past several days. She exercises daily by running on trails close to her home. She is 163 cm (5 ft 4 in) tall and weighs 58 kg (128 lb); BMI is 22 kg/m2. Temperature is 36.5°C (97.7°F), pulse is 58/min, respirations are 16/min, and blood pressure is 108/62 mm Hg. A photograph of the right arm is shown; similar findings are present on the left arm and both hands. Which of the following is the most likely primary mediator of this patient’s symptoms?
CorrectIncorrect -
Question 45 of 50
45. Question
An 82-year-old man is brought to the emergency department from the independent-living center where he resides because of a 1-day history of worsening lower abdominal pain and leakage of urine on awakening this morning. He is independent in his activities of daily living and had felt well previously. He initially attributed his abdominal pain to constipation and took milk of magnesia, which resulted in minimal bowel movement but no improvement in his symptoms. He also reports a 4-month history of occasional urinary hesitancy and nocturnal frequency. Medical history is notable for hypertension. He says he has not been evaluated by a physician “in years” and takes no medications. He does not smoke cigarettes or drink alcoholic beverages. He appears to be in mild distress. Temperature is 37.0°C (98.6°F), pulse is 90/min and regular, respirations are 16/min, and blood pressure is 170/90 mm Hg. Lungs are clear to auscultation. Palpation of the abdomen shows a tender, firm mass extending from the suprapubic region to the umbilicus area and measuring 11 cm in width. There is no edema of the extremities. The remainder of the examination shows no abnormalities. Results of dipstick urinalysis are shown:
Nitrites
Negative
WBCs
Negative
RBCs
4+
Test of the stool for occult blood is negative. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 46 of 50
46. Question
A 26-year-old man, who has been recovering in the hospital since undergoing a laparoscopic appendectomy 6 hours ago, is now being evaluated because of mild shortness of breath and dizziness upon standing. Medical history otherwise is unremarkable. Oxycodone therapy was initiated on admission, but the patient takes no routine medications. He does not drink alcoholic beverages or use illicit drugs. The patient appears pale and anxious. Vital signs are temperature 36.9°C (98.5°F), pulse 95/min, respirations 20/min, and blood pressure 88/50 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 99%. Cardiopulmonary examination discloses no abnormalities. Palpation of the abdomen discloses mild tenderness of the right lower quadrant and at the incision sites. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 47 of 50
47. Question
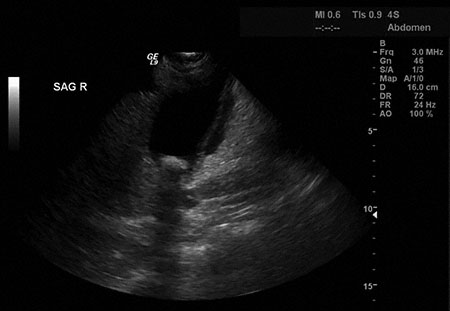
A 38-year-old woman is brought to the emergency department because of a 5-hour history of severe upper midabdominal pain, nausea, and vomiting. She rates the pain as an 8 on a 10-point scale. She has vomited three times since the onset of the pain; the vomit did not contain blood. She has had two similar episodes during the past 3 months but they were less severe and resolved without treatment. She has no history of serious illness. The patient does not use any medications. She drinks one glass of wine weekly but does not smoke cigarettes; she does not use any other substances. BMI is 25 kg/m2. Temperature is 38.7°C (101.7°F), pulse is 102/min, respirations are 16/min, and blood pressure is 136/84 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 98%. The patient is lying down and appears to be in pain. Abdominal examination discloses tenderness to palpation over the epigastric region and right upper quadrant. The tenderness is more severe with palpation while the patient is breathing deeply. The remainder of the physical examination discloses no abnormalities. Results of laboratory studies are shown:
Serum
Alkaline phosphatase
67 U/L
Bilirubin, Total
0.5 mg/dL
Blood
WBC
15,200/mm3
Neutrophils, segmented
87%
Lymphocytes
13%
Abdominal ultrasonography is shown. After administering hydration with 0.9% saline and pain control with morphine sulfate, which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 48 of 50
48. Question
A 35-year-old primigravid woman at 11 weeks’ gestation comes to the emergency department because of a 4-hour history of vaginal bleeding and pelvic pain. She had severe cramping and bleeding at home, with passage of a golf ball–sized clot; the bleeding and cramping have markedly improved since the clot passed. Two weeks ago, pelvic ultrasonography showed an intrauterine pregnancy with a fetal heart rate of 160/min, but she has not yet established routine prenatal care. Medical history is remarkable for hypothyroidism. Current medications are levothyroxine and a prenatal vitamin. Temperature is 36.8°C (98.2°F), pulse is 72/min, respirations are 14/min, and blood pressure is 124/76 mm Hg. She appears tearful. Abdominal examination shows no abnormalities. Pelvic examination shows a closed cervix with a small amount of bleeding from the cervical os. Urine pregnancy test result is positive. Pelvic ultrasonography shows no intrauterine pregnancy; there is a small amount of blood in the uterus and normal-appearing adnexa. Which of the following laboratory studies is most appropriate to obtain at this time?
CorrectIncorrect -
Question 49 of 50
49. Question
A 67-year-old man comes to the office for an annual health maintenance examination. He reports no symptoms. Medical history is remarkable for hypertension treated with lisinopril and chlorthalidone. His most recent colonoscopy at age 56 years showed no abnormalities; serum prostate-specific antigen (PSA) concentration at that time was 0.5 ng/mL (N<4.0). He smoked one-half pack of cigarettes daily for 3 years but quit 44 years ago. He drinks one to two beers twice weekly. He does not use illicit drugs. He works as a banker. He is married and is monogamous with his wife. He has four children who are healthy, and four grandchildren. He received a tetanus-diphtheria-acellular-pertussis (Tdap) vaccine 5 years ago when his first grandchild was born. The patient is 180 cm (5 ft 11 in) tall and weighs 82 kg (180 lb); BMI is 25 kg/m2. Temperature is 36.6°C (97.8°F), pulse is 68/min, respirations are 12/min, and blood pressure is 125/78 mm Hg. Physical examination discloses no abnormalities. In addition to repeat colonoscopy, which of the following is the most appropriate next step?
CorrectIncorrect -
Question 50 of 50
50. Question
A 52-year-old woman comes to an urgent care center in Denver, Colorado, because of a 1-day history of intermittent nose bleeds. She has no other history of abnormal bleeding and is otherwise asymptomatic. She has hypertension and hyperlipidemia. Her medications are lisinopril and simvastatin. She has smoked one pack of cigarettes daily for 25 years. She drinks two glasses of wine daily. She does not use illicit drugs. Temperature is 36.4°C (97.6°F), pulse is 85/min, respirations are 18/min, and blood pressure is 156/78 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 98%. On examination, the turbinates appear bloody. There are no nasal masses or ulcerations. The nasal septum is intact. The remainder of the examination shows no abnormalities. Results of laboratory studies are shown:
Hemoglobin
14.2 g/dL
Platelet count
220,000/mm3
Prothrombin time
12 sec (INR=1.0)
Partial thromboplastin time
24 sec
Which of the following factors in this patient’s history most increased her risk for developing this condition?
CorrectIncorrect
