NBME 16 – Block 3
Quiz Summary
0 of 50 Questions completed
Questions:
Information
You have already completed the quiz before. Hence you can not start it again.
Quiz is loading…
You must sign in or sign up to start the quiz.
You must first complete the following:
Results
Results
0 of 50 Questions answered correctly
Your time:
Time has elapsed
You have reached 0 of 0 point(s), (0)
Earned Point(s): 0 of 0, (0)
0 Essay(s) Pending (Possible Point(s): 0)
Categories
- Not categorized 0%
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- Current
- Review
- Answered
- Correct
- Incorrect
-
Question 1 of 50
1. Question
A 20-year-old man is brought to the emergency department immediately after being ejected from a motor vehicle during a high-speed collision. He was awake and responsive to questions at the scene. He became obtunded en route to the hospital and was intubated. On arrival, he responds only to painful stimuli. Temperature is 37.0°C (98.6°F), pulse is 100/min, respirations are 30/min and shallow, and palpable systolic blood pressure is 80 mm Hg. Pupils are equal in size. Examination shows an abrasion on the right side of the chest. There are no other external signs of trauma. Breath sounds are absent on the right. Intravenous fluid therapy is begun. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 2 of 50
2. Question
A 35-year-old woman comes to the emergency department because she has not had a menstrual period for 3 months. Results of two home pregnancy tests during this time have been negative. She has bipolar disorder accompanied by anxiety and was prescribed a new medication by her psychiatrist for her bipolar disorder 5 months ago. She is unable to recall the name of the new medication. Vital signs are within normal limits. Physical examination shows no abnormalities. She appears agitated but is cooperative and cordial. Laboratory studies show a serum prolactin concentration of 70 ng/mL (N<25). This patient was most likely prescribed which of the following drugs?
CorrectIncorrect -
Question 3 of 50
3. Question
A 30-year-old primigravid woman at 8 weeks’ gestation comes to the office because of a 3-week history of excessive sweating, difficulty sleeping, and unintentional 2-kg (4-lb) weight loss. She receives routine prenatal care. She has no history of serious illness, and her only medication is a prenatal vitamin; she does not use any other substances. Temperature is 37.0°C (98.6°F), pulse is 85/min, respirations are 18/min, and blood pressure is 128/74 mm Hg. Physical examination shows a blank stare and lid lag. Neurologic examination shows brisk deep tendon reflexes in the upper and lower extremities and proximal weakness. There is a fine resting tremor in both hands. Laboratory studies show a TSH concentration of less than 0.05 μU/mL and a free thyroxine (FT4) concentration of 6.0 ng/dL. It is most appropriate for the patient to begin taking which of the following medications at this time?
CorrectIncorrect -
Question 4 of 50
4. Question
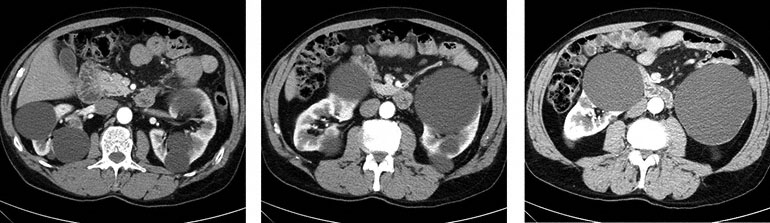
A 55-year-old man comes to the emergency department 1 hour after the sudden onset of severe left abdominal and flank pain; he also has had blood in his urine during this period. He has not had fever, chills, or difficulty with urination. His family history is unknown because he was adopted. He appears to be in pain. Temperature is 37.2°C (99.0°F), pulse is 110/min, and blood pressure is 140/100 mm Hg. Pulmonary and cardiac examinations disclose no abnormalities. Abdominal examination discloses a palpable, tender mass in the left upper quadrant and a mass in the right upper quadrant. Serum studies show a creatinine concentration of 2.4 mg/dL. CT scans of the abdomen are shown. This patient is at greatest risk for which of the following?
CorrectIncorrect -
Question 5 of 50
5. Question
A 47-year-old woman comes to the physician because of a 3-month history of shortness of breath on exertion and swelling of her ankles. She has a 22-year history of hypertension and a 2-year history of iron deficiency anemia due to menorrhagia. Current medications are hydrochlorothiazide, atenolol, lisinopril, and ferrous sulfate. Her temperature is 36.9°C (98.4°F), pulse is 88/min, respirations are 16/min, and blood pressure is 148/88 mm Hg. Jugular venous pressure is 10 cm H2O. Crackles are heard at both lung bases. There is pitting edema of the lower extremities to the knees. Her hemoglobin concentration is 10.2 g/dL, and serum creatinine concentration is 1.2 mg/dL. Echocardiography shows a thickened left ventricular wall and a decrease in early diastolic mitral flow velocity. Which of the following is the most likely cause of this patient’s edema?
CorrectIncorrect -
Question 6 of 50
6. Question
Patient Information
Age: 78 years
Gender: M, self-identified
Race/Ethnicity: Asian American, self-identified
Site of Care: clinic
History
Reason for Visit/Chief Concern: “I have a productive cough that won’t go away.”
History of Present Illness:
• 2-week history of progressive cough productive of whitish sputum
• cough worsens when eating food or drinking fluids and is associated with shortness of breath on mild exertion
• 2-day history of low-grade fever with temperatures to 37.9°C (100.3°F)
• 3-day history of increased fatigue
• no orthopnea or chest pain
• at baseline, ambulates with walker and requires assistance with bathing, dressing, and medication administration
Past Medical History:
• Parkinson disease
• benign prostatic hyperplasia
• orthostatic hypotension
• major depressive disorder
• recurrent falls
• mild cognitive impairment
Medications:
• carbidopa-levodopa
• tamsulosin
• fludrocortisone
• venlafaxine
Vaccinations:
• influenza annually
• pneumococcal 23-valent polysaccharide (PPSV23) at age 65 years
Allergies:
• no known drug allergies
Family History:
• mother: deceased at age 90 years; had dementia
• father: deceased at age 82 years from coronary artery disease
Psychosocial History:
• drinks one glass of wine every evening with dinner
• does not smoke cigarettes or use other substances
• retired artist; lives at home with his spouse
• receives assistance from a caregiver 8 hours daily
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
38.0°C
90/min
18/min
101/59 mm Hg
96%
188 cm
73 kg
21 kg/m2
(100.4°F)
on RA
(6 ft 2 in)
(160 lb)
• Appearance: frail, acutely ill; alert; not in respiratory distress; speaks in a soft voice
• Skin: no pallor
• HEENT: normocephalic, atraumatic, PERRLA; anicteric conjunctivae
• Neck: no jugular venous distention
• Pulmonary: decreased breath sounds and crackles in right lower lung base; breath sounds normal elsewhere
• Cardiac: regular S1 and S2; no S3 or murmurs
• Abdominal: soft; nontender to palpation; no organomegaly
• Extremities: no pedal edema
• Neurologic: fully oriented; increased muscle tone and rigidity in all extremities; resting tremor of hands, more prominent on the right than the left
Question: Which of the following is the most appropriate diagnostic study at this time?
CorrectIncorrect -
Question 7 of 50
7. Question
A 72-year-old woman comes to the clinic because of a 6-month history of “feeling down.” During this time, she has had no appetite, resulting in a 19-kg (42-lb) weight loss. She also has had low energy and has not been motivated to begin tasks that she should complete around her home. She says she used to enjoy going to bars with friends but she now prefers to stay home. She has also noted that her alcohol consumption has increased. During the past few years, she had been drinking one glass of wine each evening; now, she drinks two or three glasses. The patient does not use nicotine products or other substances. She has an 8-month history of low back pain, for which she takes over-the-counter pain medications, usually buying “whatever is on sale.” She takes no other medications. She is 168 cm (5 ft 6 in) tall and weighs 66 kg (146 lb); BMI is 24 kg/m2. Vital signs are within normal limits. Physical examination discloses back tenderness when she bends at the waist. On mental status examination, she reports a “sad” mood and has a congruent affect. The physician prescribes appropriate medication for the patient’s depression and related symptoms. It is most appropriate to counsel this patient about her alcohol use as well as which of the following?
CorrectIncorrect -
Question 8 of 50
8. Question

A 54-year-old woman comes to the office because of a 2-year history of gradually enlarging patches of discoloration on her hands. There is no itching or pain. She says she has not been using new soaps or lotions. Physical examination shows the findings in the photograph. It is most appropriate for the physician to evaluate this patient for the presence of which of the following additional conditions?
CorrectIncorrect -
Question 9 of 50
9. Question
A 32-year-old woman, gravida 1, para 1, comes to the office because of a 2-day history of foul-smelling vaginal discharge. One week ago, she underwent forceps-assisted vaginal delivery of a newborn at 38 weeks’ gestation. Delivery was complicated by a deep vaginal sulcus laceration that was repaired in the delivery room. Vital signs are within normal limits. Examination shows a retained surgical sponge, which is removed. The physician alerts the patient to the finding and irrigates the laceration, which appears intact. No surrounding infection is noted. Delivery was performed by one of the physician’s partners. In addition to apologizing to the patient, which of the following is the most appropriate next step by the physician?
CorrectIncorrect -
Question 10 of 50
10. Question
Patient Information
Age: 64 years
Gender: M, self-identified
Race/Ethnicity: White, self-identified
Site of Care: office
History
Reason for Visit/Chief Concern: “I’m feeling very tired.”
History of Present Illness:
• 6-month history of gradually worsening fatigue
• 5-month history of difficulty concentrating with difficulty completing his work
• sleeps 8 hours nightly, does not snore
• used to enjoy jogging for exercise but lately does not have the energy
• has never experienced these symptoms previously
Past Medical History:• no serious illnesses
Medications:
• none
Vaccinations:
• COVID-19
• influenza
Allergies:
• no known drug allergies
Psychosocial History:
• does not drink alcoholic beverages, smoke cigarettes, or use other substances
• married, lives with his spouse; has two adult children
• works as a civil engineer
• enjoys playing golf and jogging
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
37.1°C
76/min
13/min
142/79 mm Hg
100%
178 cm
77 kg
24 kg/m2
(98.7°F)
on RA
(5 ft 10 in)
(170 lb)
• Appearance: well developed, well nourished; not in acute distress
• Skin: warm and dry; no rashes
• HEENT: normocephalic, atraumatic; ocular movements full;
PERRLA; tympanic membranes gray; ear canals clear; oropharynx pink
• Neck: supple; no thyromegaly; no lymphadenopathy
• Pulmonary: clear to auscultation
• Cardiac: regular rhythm; normal S1 and S2; no murmurs, rubs, or gallops
• Abdominal: soft; nontender; no masses; no hepatosplenomegaly
• Extremities: warm and well perfused; pedal pulses 2+ bilaterally
• Neurologic: no focal deficits
Diagnostic Studies
Serum
Erythropoietin
2.1 mIU/mL (N=3.3–17.1)
Blood
Hematocrit
55%
Hemoglobin
18.4 g/dL
MCV
84 µm3
WBC
7000/mm3
Neutrophils, segmented
60%
Neutrophils, bands
5%
Lymphocytes
25%
Monocytes
7%
Eosinophils
3%
Platelet count
398,000/mm3
Question: Which of the following is the most appropriate next step in evaluation?
CorrectIncorrect -
Question 11 of 50
11. Question
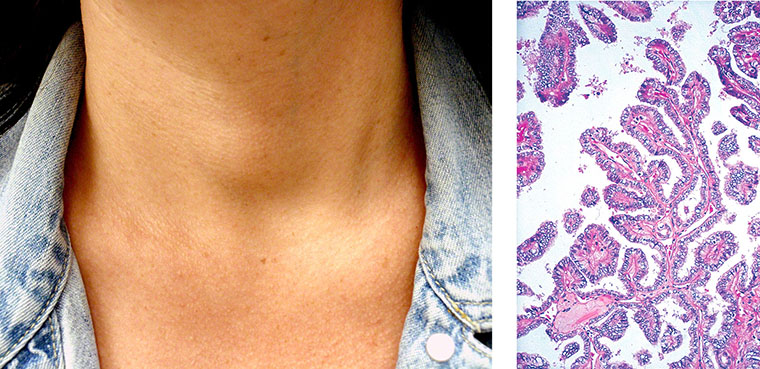
A 40-year-old woman comes to the office because of a 5-month history of a lump on the midportion of her neck. She has no history of serious illness and takes no medications. She is 168 cm (5 ft 6 in) tall and weighs 54 kg (120 lb); BMI is 19 kg/m2. Vital signs are within normal limits. A photograph of the patient is shown. Serum TSH and thyroxine (T4) concentrations are within the reference ranges; no thyroid autoantibodies are detected. A photomicrograph of an ultrasonography-guided fine-needle aspiration of the nodule also is shown. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 12 of 50
12. Question
A 68-year-old woman comes to the office for a routine follow-up examination 6 months after completing treatment for colorectal cancer. Her treatment consisted of surgical excision of the colon followed by a 6-month course of chemotherapy with leucovorin, fluorouracil, oxaliplatin, and radiation therapy. The procedure was complicated by a prolonged recovery, and she has been mostly sedentary during this time. The patient now reports a 4-week history of decreased sensation in her fingertips, as well as numbness and tingling in both feet. Medical history otherwise is unremarkable. She currently takes no medications. She is 163 cm (5 ft 4 in) tall and weighs 84 kg (185 lb); BMI is 32 kg/m2. Vital signs are within normal limits. Examination shows decreased sensation to pinprick over all fingers and toes. Which of the following is the most likely cause of this patient’s symptoms?
CorrectIncorrect -
Question 13 of 50
13. Question
A 36-year-old man comes to the office because of a 3-month history of a firm, intermittently painful lump in his groin. He first noticed the lump while he was lifting weights and it continues to bother him daily. He has not sustained recent trauma to the area. He has no history of serious illness and takes no medications. Vital signs are within normal limits. Examination shows a reducible, nontender mass in the inguinal region when the patient is standing and coughing. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 14 of 50
14. Question
A 28-year-old woman, gravida 3, para 2, at 22 weeks’ gestation comes to the office for a routine prenatal visit. Pregnancy has been complicated by major depressive disorder, diagnosed 1 year ago. Current medications are citalopram and a prenatal vitamin. Her two previous pregnancies ended in uncomplicated vaginal deliveries at term 2 and 5 years ago. She feels well and has no other history of serious illness. Her husband is currently deployed with the military, and her family lives in a different state. She is the primary caregiver for her two young children. The patient has smoked one-half pack of cigarettes daily for 5 years and has continued to smoke during pregnancy. She does not drink alcoholic beverages or use other substances. Examination shows a uterus consistent in size with a 22-week gestation. Pelvic ultrasonography shows a bilateral fetal diaphragmatic defect with abdominal contents in the fetal chest with minimal lung tissue. The patient is offered pregnancy termination and she declines. It is most appropriate for the physician to consider which of the following factors in determining newborn treatment at delivery?
CorrectIncorrect -
Question 15 of 50
15. Question
A 37-year-old man is brought to the emergency department 30 minutes after he was involved in a motor vehicle collision. He was the unrestrained driver traveling at approximately 70 mph. On arrival, he is alert. He is in mild respiratory distress and reports chest pain. His pulse is 120/min, respirations are 25/min, and blood pressure is 85/65 mm Hg. Examination discloses a steering wheel impression on the anterior chest and a nondistended, nontender abdomen. Breath sounds are clear and equal. X-ray of the chest shows fractures of ribs 4 through 8 on the right and a small pneumothorax. ECG shows sinus tachycardia, low amplitude, and multiple premature ventricular contractions. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 16 of 50
16. Question
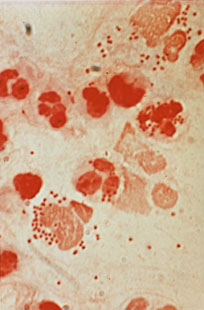
A 23-year-old woman comes to the physician because of a 1-day history of vaginal itching and mucous discharge. She had sexual intercourse with a new male partner 1 week ago, and they did not use a condom. Her temperature is 37.7°C (99.8°F). Pelvic examination shows an erythematous cervix with a purulent exudate from the cervical os. A photomicrograph of a Gram stain of the discharge is shown. In addition to ceftriaxone, which of the following is the most appropriate pharmacotherapy for this patient?
CorrectIncorrect -
Question 17 of 50
17. Question
A 3-year-old girl is brought to the clinic by her mother for a well-child examination. Her mother reports no concerns. Medical history is unremarkable and she receives no medications. Vaccinations are up-to-date. She is at the 50th percentile for height and weight; BMI is at the 55th percentile. Temperature is 37.6°C (99.7°F), pulse is 120/min, respirations are 22/min, and blood pressure is 90/64 mm Hg. Pupils are equal, round, and reactive to light. Retinal reflex is present bilaterally. Photo vision screening discloses anisometropia with hyperopia that is greater in the right eye than the left. Without treatment, this patient is at increased risk for developing which of the following complications?
CorrectIncorrect -
Question 18 of 50
18. Question
A 58-year-old woman, who is a military conflict veteran, comes to the Veterans Affairs clinic because of a 3-day history of watery diarrhea accompanied by cramping abdominal pain. She has been having 10 to 12 bowel movements daily and has awakened from sleep to use the bathroom. She also has had fever, nausea, and loss of appetite during this time. She has not had vomiting or blood in her stool. She has hypertension and gastroesophageal reflux disease. Two weeks ago she had a urinary tract infection treated with a 3-day course of trimethoprim-sulfamethoxazole. Routine medications are amlodipine and omeprazole. Temperature is 38.0°C (100.4°F), pulse is 92/min, respirations are 12/min, and blood pressure is 138/82 mm Hg. Examination of the extremities shows no edema or skin lesions. The mucous membranes are dry. There is no pharyngeal erythema. Cardiopulmonary examination discloses no abnormalities. The abdomen is soft and mildly distended with diffuse tenderness in the lower quadrants bilaterally. Bowel sounds are increased. Which of the following is the most appropriate next step in diagnosis?
CorrectIncorrect -
Question 19 of 50
19. Question
A 22-year-old man comes to the office because of a 6-day history of blood-tinged urine, especially in the morning. He also has felt much more tired than usual during the past week, which he attributes to training for his first 5K run, and has had difficulty swallowing during the past 3 days. He has no history of serious illness and takes no medications. Temperature is 37.1°C (98.7°F), pulse is 105/min, respirations are 30/min, and blood pressure is 120/72 mm Hg. Physical examination discloses pallor and mild splenomegaly. No other abnormalities are noted. A complete blood count with differential indicates the presence of Coombs-negative hemolytic anemia. Based on the suspected diagnosis, peripheral blood flow cytometry is ordered, which indicates deficiency of glycosylphosphatidylinositol (GPI)-anchoring proteins. This patient is at greatest risk for which of the following?
CorrectIncorrect -
Question 20 of 50
20. Question
A 17-year-old girl comes to the office for an examination prior to attending college where she will play on the school’s lacrosse team. She feels well. She has no history of serious illness and takes no medications. Menarche was at the age of 12 years. Menses occur at regular 26-day intervals with moderate flow. Her mother and father have hypertension, and her father has type 1 diabetes mellitus. The patient receives grades of A’s and B’s in school. She has been sexually active with her boyfriend for the past 6 months; they use cycle awareness and the withdrawal method for contraception. She does not smoke cigarettes, drink alcoholic beverages, or use other substances. Today, she will receive the last dose of the human papillomavirus vaccine series; other vaccinations are up-to-date. She is at the 45th percentile for height, 80th percentile for weight, and 80th percentile for BMI. Vital signs are within normal limits. Examination discloses no abnormalities. In addition to providing comprehensive contraceptive counseling, which of the following is the most appropriate screening test for this patient at this time?
CorrectIncorrect -
Question 21 of 50
21. Question
An 18-year-old woman is brought to the emergency department via ambulance 25 minutes after she sustained injuries during a motor vehicle collision in which her automobile was struck head-on by another vehicle. She was the restrained driver, and her airbag deployed. She was found unconscious in the wreckage and was extracted by paramedics. En route, she received advanced cardiac life support measures, including defibrillation and epinephrine. She was intubated and stabilized. On arrival, she is unresponsive. Temperature is 36.0°C (96.8°F), pulse is 95/min, respirations are 17/min, and blood pressure is 100/70 mm Hg. Physical examination shows severe bruising over the sternum. Bilateral crackles are heard. There is evidence of a right hip fracture but no evidence of head trauma. Transthoracic echocardiography shows severe mitral valve regurgitation. The patient’s blood pressure decreases to 90/40 mm/Hg, and there is atrial fibrillation and subsequent asystole. Despite appropriate intervention, the patient dies. Which of the following is the most likely cause of this patient’s death?
CorrectIncorrect -
Question 22 of 50
22. Question
A state legislator plans to introduce a bill to eliminate a current law requiring that all motorcycle drivers wear helmets. The state public health association is lobbying against the bill, citing many studies supporting the use of motorcycle helmets for prevention of head trauma sustained in motor vehicle collisions involving motorcycles. Which of the following best describes the level of prevention mentioned in the studies cited by the state’s public health association?
CorrectIncorrect -
Question 23 of 50
23. Question
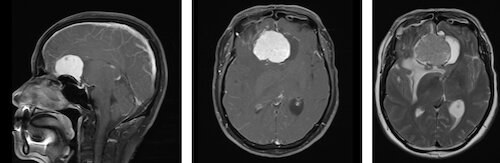
A 65-year-old man comes to the office with this wife because of a 6-month history of increasingly severe headache accompanied by nausea. His wife says his personality has changed, and that he has been more apathetic during this period. He has no personal or family history of serious illness and does not use medications or other substances. Temperature is 37.0°C (98.6°F), pulse is 72/min, respirations are 16/min, and blood pressure is 125/80 mm Hg. He is awake and alert. Neurologic examination discloses optic atrophy in the right eye, papilledema in the left eye, and anosmia. The remainder of cranial nerve testing shows no abnormalities. Muscle strength is 5/5 in the upper and lower extremities bilaterally. Sensation to light touch, pinprick, and proprioception is intact. There are no cerebellar abnormalities and he walks with a normal gait. He is oriented to person, place, and time. MRIs of the brain with contrast are shown. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 24 of 50
24. Question
A 32-year-old primigravid woman at 28 weeks’ gestation comes to the emergency department 3 hours after an episode of bright red vaginal bleeding. Her pregnancy otherwise has been uncomplicated. She has no history of serious illness. Vital signs are within normal limits. Examination shows a uterus consistent in size with a 28-week gestation; the fetus is in a floating breech presentation. Ultrasonography shows a partial placenta previa with a normal volume of amniotic fluid. The fetus is consistent in size with a 28-week gestation. She is admitted to the hospital for observation. During the next 24 hours, there is no further bleeding, and the fetal status remains reassuring. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 25 of 50
25. Question
A 27-year-old primigravid woman at 28 weeks’ gestation comes to the emergency department 3 hours after the onset of contractions. She has had no vaginal bleeding and has not had sexual intercourse recently. Her pregnancy had been uncomplicated. External fetal monitoring shows contractions every 3 minutes; the fetal heart rate is reassuring. Speculum examination shows no abnormalities. There is no blood in the vaginal vault. The membranes are intact. A fetal fibronectin assay (FFN) from the posterior vagina is negative. Digital examination shows a long, closed cervix. The physician informs the patient that her risk for delivery within the next 2 weeks is less than 1%. Which of the following factors makes FFN the most appropriate test for predicting the risk of preterm delivery in this patient?
CorrectIncorrect -
Question 26 of 50
26. Question
An 83-year-old woman comes to the clinic because of a 1-year history of progressive shaking of both hands. The shaking is more pronounced with the right hand, particularly when she tries to hold an object or write. Her spouse has noted that her head also shakes intermittently. She has had no recent falls or changes in gait. Medical history is remarkable for essential hypertension, hypothyroidism, osteoarthritis of both knees, and major depressive disorder. Medications are hydrochlorothiazide, levothyroxine, and sertraline. She uses a four-wheeled walker for ambulation and is independent in all other activities of daily living. Family history is remarkable for Parkinson disease in her paternal grandfather. The patient occasionally drinks alcoholic beverages. She uses no other substances. She is 175 cm (5 ft 9 in) tall and weighs 61 kg (135 lb); BMI is 20 kg/m2. Temperature is 36.5°C (97.7°F), pulse is 82/min and regular, respirations are 16/min, and blood pressure is 132/65 mm Hg. The patient is alert and fully oriented. Muscle tone is normal and muscle strength is 5/5. Coordination testing discloses fast, repetitive shaking of the fingers and a side-to-side motion of the head. Gait is stable when ambulating with the walker. Which of the following is the most likely cause of these findings?
CorrectIncorrect -
Question 27 of 50
27. Question
Three days after discharge following uncomplicated total abdominal hysterectomy and bilateral salpingo-oophorectomy for management of ovarian cancer, a 57-year-old woman comes to the emergency department because of a 3-hour history of progressive dyspnea and increasingly severe chest pain. She has no other history of serious illness and took no medications prior to admission. At the time of discharge, she was prescribed hydrocodone-acetaminophen. She does not smoke cigarettes. Temperature is 37.0°C (98.6°F), pulse is 112/min, respirations are 32/min, and blood pressure is 118/78 mm Hg. There is a clean, intact surgical incision over the abdomen. The remainder of the examination shows no abnormalities. Results of laboratory studies are shown:
Serum
Creatinine
0.6 mg/dL
Creatine kinase
63 U/L
Blood
Hematocrit
37.5%
Hemoglobin
12.5 g/dL
WBC
12,340/mm3
Neutrophils, segmented
69%
Bands
6%
Lymphocytes
25%
Results of arterial blood gas analysis on 2 L/min of oxygen by nasal cannula are shown:
Po2
65 mm Hg
Pco2
30 mm Hg
pH
7.48
O2 saturation
94
12-Lead ECG shows sinus tachycardia. Chest x-ray shows no abnormalities. CT scan of the chest shows a filling defect in one of the branches of the right pulmonary artery. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 28 of 50
28. Question
An 18-month-old boy is brought to the emergency department because of a 2-day history of temperatures to 38.9°C (102.0°F). During the past 6 months, he has had four episodes of otitis media that resolved with amoxicillin therapy. He currently receives no medications. Immunizations are up-to-date. The patient is at the 10th percentile for length, weight, and head circumference. Temperature is 39.4°C (103.0°F), pulse is 130/min, and respirations are 36/min. Examination of the left knee shows swelling, erythema, and tenderness to palpation. Leukocyte count is 10,000/mm3 (N=6000–14,000), and absolute neutrophil count is 480/mm3 (N>500). Serum immunoglobulin concentrations are decreased, and B lymphocytes are absent. Culture of fluid aspirated from the knee grows Streptococcus pneumoniae, and the patient’s symptoms improve with intravenous ceftriaxone therapy. The patient’s mother reports that her maternal great uncle died of sepsis as a child. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 29 of 50
29. Question
A 1-week-old girl is brought to the office by her father for a well-child examination. She has no history of serious illness and receives no medications. Vaccinations are up-to-date. She was born at 39 weeks’ gestation to a 29-year-old woman, gravida 1, para 1, following uncomplicated spontaneous vaginal delivery. Growth and development have been normal. She is 50 cm (20 in; 50th percentile) long and weighs 3400 g (7 lb 8 oz; 50th percentile); head circumference is 34.2 cm (13.5 in; 50th percentile). Vital signs are within normal limits. Examination discloses instability of the right hip on flexion when posterior pressure is applied to the femur. No other abnormalities are noted. Ultrasonography of the hips confirms the diagnosis. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 30 of 50
30. Question
A 3-year-old girl is brought to the urgent treatment center by her father because of a 3-week history of rash on her face and buttocks; the rash is not itchy or painful. The father says they have not recently changed bath soaps or laundry detergents and have not begun eating any new foods recently. The patient is otherwise asymptomatic. She has no history of serious illness and receives no medications. The father says his daughter is a “very picky eater.” Vital signs and oxygen saturation are within normal limits. Examination shows a perioral rash with mild edema and erythema. The rash on the buttocks is more erythematous, but there are no satellite lesions or other signs of infection. The remainder of the examination discloses no abnormalities. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 31 of 50
31. Question
A 16-year-old boy is brought to the clinic because of a 3-month history of a 9.1-kg (20-lb) weight gain that he attributes to increased eating. His mother died in a motor vehicle collision 6 months ago. Since then, he says it takes him an hour to fall asleep, he wakes up at 4 am every morning, and he lies in bed not wanting to get out. He spends most of the day in his bedroom. He has missed 4 weeks of school and is failing some classes. He was an avid wrestler but is not participating this year. He says, “I just don’t care about anything. Eating is the only thing that seems to help.” He snacks throughout the day and has been eating double his normal portions at meals. He feels guilty about his increased eating and has been inducing vomiting four times weekly “so I don’t get fat.” He has been attending individual and family therapy during the past 4 months. He has no history of serious illness and takes no medications. He does not use nicotine products, drink alcohol, or use other substances. He is at the 25th percentile for height, 70th percentile for weight, and 84th percentile for BMI. Vital signs are within normal limits. He makes poor eye contact during the visit. Physical examination discloses no abnormalities. On mental status examination, he has a blunted and dysphoric affect and describes his mood as “whatever.” He has no suicidal ideation or thoughts of self harm. Which of the following is the most appropriate pharmacotherapy at this time?
CorrectIncorrect -
Question 32 of 50
32. Question
A hospitalized 46-year-old woman undergoes uncomplicated vaginal hysterectomy and bilateral salpingo-oophorectomy for leiomyoma uteri and heavy menstrual bleeding. Estimated blood loss is 100 mL. Immediately following the operation, cystoscopy shows an intact bladder, a brisk urine jet from the left ureteral orifice, and no urine jet from the right ureteral orifice. Which of the following operative steps is the most likely cause of the cystoscopy findings?
CorrectIncorrect -
Question 33 of 50
33. Question
Physicians at an outpatient clinic would like to increase the percentage of patients with type 2 diabetes mellitus treated in the clinic who undergo recommended annual diabetic foot examination. The baseline percentage of patients with type 2 diabetes mellitus in this patient population who underwent diabetic foot examination during the past year was 30%. The clinic would like to improve this number to greater than 70% during the next 6 months. Which of the following measurement tools is most appropriate for the physicians to track their progress?
CorrectIncorrect -
Question 34 of 50
34. Question
A 45-year-old woman comes to the clinic to discuss the results of fiberoptic bronchoscopy performed 2 days ago for evaluation of a 6-month history of a progressively worsening cough. She was initially seen in the clinic 10 days ago after she had three episodes of blood-streaked sputum in 3 days. Chest x-ray and CT scan of the chest obtained at the initial visit showed a 2.5-cm centrally located opacity in the right upper lobe. Today, the patient says she feels well. Medical history is remarkable for hypertension; she underwent a hysterectomy 3 years ago for leiomyomata uteri. Her only medication is hydrochlorothiazide. The patient does not smoke cigarettes, drink alcoholic beverages, or use other substances. She is 170 cm (5 ft 7 in) tall and weighs 68 kg (150 lb); BMI is 24 kg/m2. Temperature is 37.0°C (98.6°F), pulse is 75/min, respirations are 12/min, and blood pressure is 120/80 mm Hg. Physical examination discloses no abnormalities. Results of fiberoptic bronchoscopy show an endobronchial mass. Biopsy of the mass confirms the diagnosis. The mass is well differentiated. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 35 of 50
35. Question
A 62-year-old man comes to the office because of increasing difficulty achieving an erection during the past 2 years; for 2 months, he has been unable to achieve an erection. Two years ago, he noted that he had no semen discharge with orgasm. He has a 13-year history of hypertension treated with lisinopril and a 20-year history of type 2 diabetes mellitus treated with metformin. He also takes atorvastatin. Pulse is 90/min, respirations are 16/min, and blood pressure is 155/92 mm Hg while sitting and 130/80 mm Hg while standing. Lungs are clear to auscultation. An S4 gallop is heard; there are no murmurs. Pedal pulses are intact. Prostate is symmetrically enlarged; there is no tenderness or nodules. Proprioception and sensation to vibration and light touch are decreased to the knees bilaterally. Ankle reflexes are absent bilaterally. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 36 of 50
36. Question
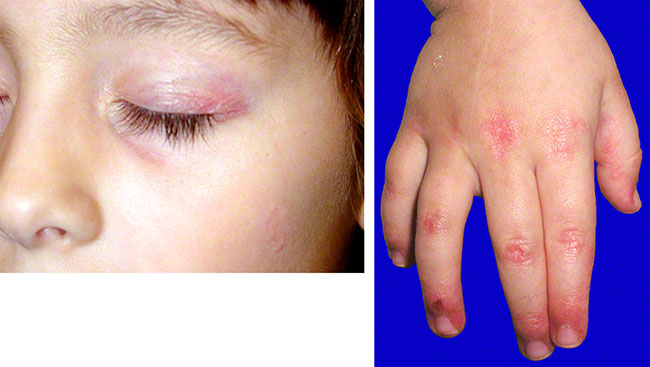
A 7-year-old girl is brought to the office by her parents because of a 7-week history of intermittent fever, joint pain, malaise, and an unintentional 2-kg (5-lb) weight loss, despite no change in appetite. She also has had progressive difficulty rising from a chair and walking up stairs during this time. Medical history is unremarkable. She takes no medications and has never been hospitalized. She is at the 50th percentile for height and 25th percentile for weight. Vital signs are normal except for a temperature of 38.0°C (100.4°F). Physical examination discloses the findings shown in the photographs. Muscle strength is 3/5 in the proximal aspects of the upper and lower extremities. When asked to walk across the examination room, the patient appears to walk on her toes. Which of the following is the most appropriate next step in diagnosis?
CorrectIncorrect -
Question 37 of 50
37. Question
A 42-year-old man comes to the urgent care center because of a 1-month history of constipation and rectal bleeding. He says he has had to strain in order to have a bowel movement on most days. During this time, he has noticed bright red blood both on the toilet paper and streaking in his stools. Medical history is unremarkable and he takes no medications. He does not use other substances. Family history is unremarkable. The patient self-identifies as African American. He is 185 cm (6 ft 1 in) tall and weighs 90 kg (198 lb); BMI is 26 kg/m2. Vital signs are within normal limits. The patient appears well. Cardiopulmonary examination discloses no abnormalities. Abdomen is soft and nontender. Rectal examination shows multiple hemorrhoids with no active bleeding. Results of laboratory studies are shown:
Serum
Na+
139 mEq/L
K+
4.1 mEq/L
Cl−
100 mEq/L
HCO3−
23 mEq/L
Urea nitrogen
23 mg/dL
Creatinine
1.0 mg/dL
Glucose, random
85 mg/dL
Blood
Hematocrit
38%
Hemoglobin
12.5 g/dL
MCV
72 µm3
WBC
10,000/mm3
Platelet count
250,000/mm3
Urine
Blood
Negative
Leukocyte esterase
Negative
WBCs
0/hpf
RBCs
0/hpf
Toxicology screen
Negative
In addition to treating the patient’s hemorrhoids, which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 38 of 50
38. Question
Twenty-four hours after undergoing laparotomy for appendicitis, a 2-year-old girl receives morphine for pain management. Fifteen minutes later, she is somnolent. Her pulse is 80/min, respirations are 15/min, and blood pressure is 80/50 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 60%. The patient is administered naloxone and immediately awakens; pulse oximetry on room air now shows an oxygen saturation of 100%, and all vital signs are within normal limits. A root cause analysis of this adverse event should be designed to examine which of the following?
CorrectIncorrect -
Question 39 of 50
39. Question
A 58-year-old woman comes to the office because of a 1-day history of pain and redness of her right great toe. She says the pain woke her from sleep last night. She rates the pain as a 7 on a 10-point scale. She has not had fever and there is no discharge from the toe. The patient has never had a similar episode in the past. She has not recently changed her diet. Medical history is remarkable for hypertension, hyperlipidemia, and osteoarthritis. Medications are losartan, hydrochlorothiazide, simvastatin, ezetimibe, and acetaminophen. She does not smoke cigarettes, drink alcoholic beverages, or use other substances. She is 160 cm (5 ft 3 in) tall and weighs 61 kg (135 lb); BMI is 24 kg/m2. Vital signs are within normal limits. Physical examination shows erythema, warmth, and tenderness to palpation at the metatarsophalangeal joint of the right great toe. Analysis of fluid aspirated from the right great toe is most likely to show which of the following?
CorrectIncorrect -
Question 40 of 50
40. Question
Patient Information
Age: 47 years
Gender: F, self-identified
Race/Ethnicity: unspecified
Site of Care: clinic
History
Reason for Visit/Chief Concern: annual health maintenance examination
History of Present Illness:
• patient has no concerns
• requests routine screening blood work
• requests renewal of allergy medication prescriptions
• says her allergies are well controlled
Past Medical History:
• allergic rhinitis
Medications:
• fluticasone
• loratadine
Vaccinations:
• up-to-date
Allergies:
• no known drug allergies
Family History:
• mother: deceased at age 78 years from stroke; hypertension
• father: deceased at age 73 years from colon cancer
Psychosocial History:
• has smoked one pack of cigarettes daily for 30 years
• does not drink alcoholic beverages or use other substances
• lives with her husband and daughter
• works as a teacher
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
36.2°C
97/min
18/min
120/80 mm Hg
98%
165 cm
63 kg
23 kg/m2
(97.1°F)
on RA
(5 ft 5 in)
(140 lb)
• Appearance: well; no acute distress
• HEENT: no conjunctival icterus; PERRLA; ocular movements intact; moist oropharynx
• Pulmonary: clear to auscultation
• Cardiac: regular rhythm; no murmurs, rubs, or gallops
• Abdominal: nondistended; soft, nontender to palpation
• Extremities: no clubbing, cyanosis, or edema
Diagnostic Studies
Serum
Na+
142 mEq/L
K+
3.9 mEq/L
Cl–
103 mEq/L
HCO3–
28 mEq/L
Urea nitrogen
13 mg/dL
Creatinine
0.64 mg/dL
Glucose, fasting
104 mg/dL
Calcium
9.7 mg/dL
ALT
16 U/L
AST
12 U/L
Cholesterol, fasting
Total
213 mg/dL
HDL
48 mg/dL
LDL
142 mg/dL
Triglycerides
115 mg/dL
Blood
Hematocrit
33%
Hemoglobin
12.0 g/dL
MCV
84.3 µm3
WBC
8000/mm3
Platelet count
254,000/mm3
• screening mammography obtained 6 months ago: no abnormalities
Question: In addition to recommending smoking cessation, which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 41 of 50
41. Question
A 32-year-old man comes to the clinic because of a 2-year history of fear that he is making inappropriate comments at work and an inability to stop worrying about them. The patient “constantly” worries that he is saying the “wrong thing,” and he routinely asks coworkers and friends if his comments at work are appropriate. He says they frequently assure him that he did not say anything inappropriate, but they describe his constant checking as “obnoxious.” The patient states that he wishes he could stop asking about his behavior, but he says “self-assurance” isn’t enough; he “needs to be sure what others are thinking” about him. He has no history of serious illness and takes no medications. Both of his parents have generalized anxiety disorder. Physical examination of the patient discloses no abnormalities. On mental status examination, the patient has good insight and repeatedly asks questions during the interview such as, “Was that offensive?,” “Did I over-share?,” and “Am I saying that right?” Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 42 of 50
42. Question
A 25-year-old man who is a veteran of the US Army comes to the office because of frequent nightmares and difficulty sleeping since he was sexually assaulted by two soldiers in his unit 3 years ago while on deployment. He says that in his nightmares, he re-experiences the assault and wakes up “sweating, with my heart beating really fast, and feeling like I was back in our old barracks.” He has not had hypervigilance or avoidance of any specific situations. He says he enjoys his current job as a music promoter and has been promoted twice during the past year. He notes he has been happily married to a supportive spouse for the past 5 years, and they hope to have children soon. He has no history of serious illness and takes no medications. He appears well, appears his stated age, and is socially engaged. Vital signs are within normal limits. Physical examination discloses no abnormalities. Mental status examination discloses a euthymic affect. Which of the following is the most appropriate pharmacotherapy at this time?
CorrectIncorrect -
Question 43 of 50
43. Question
A 24-year-old primigravid woman at 41 weeks’ gestation is admitted to the hospital in active labor. She had been laboring at home with her partner and a midwife, who recommended she come to the hospital because labor has not progressed during the past 12 hours. The patient reports that contractions have occurred every 5 to 7 minutes for the past 12 hours, with good fetal movement and no leakage of vaginal fluid. Vital signs are within normal limits. The fetus is in a vertex presentation, confirmed by bedside ultrasonography. Fetal heart tracing is category 1. Tocodynamometer shows irregular contractions every 6 to 7 minutes. The attending physician recommends artificial rupture of membranes and labor augmentation with intravenous oxytocin, requiring continuous fetal monitoring. The patient wishes to continue to try for a natural delivery with no medical interventions. Which of the following ethical principles should the physician consider to guide management at this time?
CorrectIncorrect -
Question 44 of 50
44. Question
A 22-year-old man comes to the clinic for screening for sexually transmitted infections. He is asymptomatic and says he feels well. During the past year, he has had two episodes of chlamydia. He has no other history of serious illness or known allergies. Immunizations, including for human papillomavirus, are up-to-date. Current medication is only a multivitamin. He has had 80 lifetime male and female sexual partners since the age of 18 years; he uses condoms inconsistently. He lives in an apartment with two roommates and works in a coffee shop. Vital signs are within normal limits. Physical examination discloses no abnormalities. In addition to recommending more consistent condom use, which of the following is the most effective method of HIV prevention to recommend for this patient?
CorrectIncorrect -
Question 45 of 50
45. Question
A 16-year-old girl is brought to the emergency department 3 hours after she was sexually assaulted by a male acquaintance. She says she drank five cocktails at a party, became ill, and lost consciousness. When she awoke, she was naked, her vulvovaginal area was sore, and there was blood on the bed. Menses occur at regular 28-day intervals. Her last menstrual period was 12 days ago. She was last sexually active 2 years ago. Examination shows abrasions along the posterior fourchette. The remainder of the examination shows no abnormalities. Microscopy of vaginal secretions shows motile sperm. In addition to appropriate antibiotic therapy, administration of which of the following is the most appropriate recommendation at this time?
CorrectIncorrect -
Question 46 of 50
46. Question
A 4-year-old boy is brought to the emergency department by his mother 1 hour after she found him playing with his grandfather’s medications. At the time he was found, there were pills on the floor and one empty bottle. The grandfather has hypertension, type 2 diabetes mellitus, and coronary artery disease. The grandfather’s current medications include aspirin, atorvastatin, docusate sodium, labetalol, and metformin. On arrival, the child is awake but sleepy. His temperature is 37.1°C (98.8°F), pulse is 120/min, respirations are 32/min, and blood pressure is 88/60 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 100%. Physical examination shows no other abnormalities. Results of arterial blood gas analysis are shown:
pH
7.49
Pco2
22 mm Hg
Po2
95 mm Hg
HCO3−
22 mEq/L
This patient most likely ingested which of the following medications?
CorrectIncorrect -
Question 47 of 50
47. Question
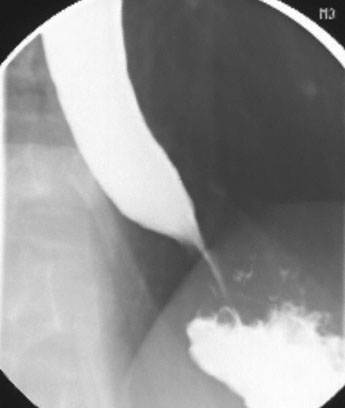
A previously healthy 47-year-old man comes to the physician because of a 3-month history of progressive difficulty swallowing, resulting in a 6-kg (13.2-lb) weight loss. During the past 2 weeks, he has had occasional regurgitation of ingested food. He has not had difficulty breathing or hoarseness. He takes no medications. He does not smoke cigarettes or drink alcohol. His temperature is 37°C (98.6°F), pulse is 75/min, respirations are 18/min, and blood pressure is 122/78 mm Hg. Examination of the neck shows no masses or lymphadenopathy. Cardiopulmonary examination shows no abnormalities. A chest x-ray shows an air-fluid level posterior to the cardiac silhouette. Results of a barium swallow are shown. Esophagogastroduodenoscopy shows esophagitis in the distal esophagus but no stricture or masses. Which of the following is most likely to confirm the diagnosis?
CorrectIncorrect -
Question 48 of 50
48. Question
Patient Information
Age: 32 years
Gender: F, self-identified
Race/Ethnicity: Guatemalan, self-identified
Site of Care: clinic
History
Reason for Visit/Chief Concern: “I’d like a check-up before I get pregnant.”
History of Present Illness:
• nulligravid
• wants evaluation before attempting to conceive with her husband
• menses occur at regular 30-day intervals
• husband uses condoms but plans to stop after this visit “if everything is okay”
Past Medical History:
• exercise-induced bronchospasm
• environmental allergies
Medications:
• albuterol inhaler prn prior to exercise
• fexofenadine prn for allergies
• multivitamin
Allergies:
• penicillin (unknown reaction)
Family History:
• mother: alive with type 2 diabetes mellitus
• father: alive with hypertension
Psychosocial History:
• immigrated to the United States from Guatemala with her husband 5 years ago
• does not smoke cigarettes, drink alcoholic beverages, or use other substances
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
36.9°C
72/min
18/min
124/76 mm Hg
—
157 cm
69 kg
28 kg/m2
(98.4°F)
(5 ft 2 in)
(152 lb)
• Appearance: well
• Skin: warm and dry
• Pulmonary: clear to auscultation; no wheezes or crackles
• Cardiac: regular rhythm; normal S1 and S2; no murmurs, rubs, or gallops
• Abdominal: nondistended; normal bowel sounds; soft; nontender
• Extremities: no edema; full range of motion
Diagnostic Studies
Blood
Hematocrit
34%
Hemoglobin
12.2 g/dL
WBC
5600/mm3
Platelet count
223,000/mm3
Question: Which of the following is the most appropriate initial step for this patient?
CorrectIncorrect -
Question 49 of 50
49. Question
An 82-year-old man is brought to the clinic because of a 6-week history of fainting with exertion. These episodes are preceded by sweating. He also has had increasingly severe chest pain and shortness of breath with exertion during the past 4 months. His last visit to a physician was 5 years ago. He has no history of serious illness and uses no medications or substances. He is 163 cm (5 ft 4 in) tall and weighs 69 kg (152 lb); BMI is 26 kg/m2. Temperature is 37.0°C (98.6°F), pulse is 90/min and regular, respirations are 15/min, and blood pressure is 150/90 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 100%. The patient is alert and fully oriented. Cardiac examination discloses a grade 3/6 crescendo-decrescendo systolic murmur that is best heard at the second right intercostal space; the murmur radiates to the carotid arteries bilaterally. S1 is normal, but S2 is not heard. Neurologic examination discloses no abnormalities. Which of the following factors in this patient’s history most strongly indicates a poor prognosis without intervention?
CorrectIncorrect -
Question 50 of 50
50. Question
Three months after treatment for pseudomonal pneumonia, a 37-year-old man comes to the physician because of a daily cough productive of copious sputum since that time. He has a history of several episodes of right lower lobe pneumonia during childhood and recurrent right lower lobe pneumonia during adulthood. He smoked two packs of cigarettes daily for 14 years but quit 7 years ago. Inspiratory crackles are heard over the right lower lobe. An x-ray of the chest shows dilated, thickened airways in the right lower lobe. Which of the following is the most likely diagnosis?
CorrectIncorrect
