NBME 16 – Block 2
Quiz Summary
0 of 50 Questions completed
Questions:
Information
You have already completed the quiz before. Hence you can not start it again.
Quiz is loading…
You must sign in or sign up to start the quiz.
You must first complete the following:
Results
Results
0 of 50 Questions answered correctly
Your time:
Time has elapsed
You have reached 0 of 0 point(s), (0)
Earned Point(s): 0 of 0, (0)
0 Essay(s) Pending (Possible Point(s): 0)
Categories
- Not categorized 0%
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- Current
- Review
- Answered
- Correct
- Incorrect
-
Question 1 of 50
1. Question
A 44-year-old woman comes to the clinic because of a 3-day history of “painful sores near my vagina.” She has no history of serious illness or similar symptoms and takes no medications. She identifies as heterosexual and reports regular unprotected vaginal intercourse with her husband of 20 years. She is 157 cm (5 ft 2 in) tall and weighs 60 kg (133 lb); BMI is 24 kg/m2. Temperature is 37.4°C (99.3°F), pulse is 90/min, respirations are 18/min, and blood pressure is 140/88 mm Hg. She appears moderately uncomfortable. Examination discloses vulvar ulcers. There is one enlarged and tender inguinal lymph node. One of the labial lesions is swabbed and submitted for further testing. Which of the following infectious agents is the most likely cause of this patient’s condition?
CorrectIncorrect -
Question 2 of 50
2. Question
A 26-year-old woman comes to the office because of a 6-month history of an increase in facial hair and occasional breakouts of acne. She has no history of serious illness. Menses have occurred at irregular 45- to 60-day intervals since menarche at the age of 8 years. Ultrasonography of the ovary 1 month ago showed no abnormalities. She takes no medications. She is 160 cm (5 ft 3 in) tall and weighs 70 kg (155 lb); BMI is 28 kg/m2. Vital signs are within normal limits. Physical examination shows increased facial and body hair, increased sebaceous secretions, and moderate clitoral enlargement. Serum studies are most likely to show an increase in which of the following?
CorrectIncorrect -
Question 3 of 50
3. Question
A 47-year-old man comes to the office for a follow-up examination 6 weeks after testing positive for hepatitis C during laboratory screening for life insurance. He has a history of osteoarthritis of the knees and takes ibuprofen, one tablet, twice daily. He does not smoke cigarettes and drinks one glass of wine four to five times weekly. He does not use intravenous drugs and has had no blood transfusions. He is sexually active and monogamous with his wife. Vital signs are within normal limits. The patient appears well. Examination shows no abnormalities. Results of liver function tests, complete blood count, and serum studies, including measurement of total cholesterol concentration, are within the reference ranges. In addition to serologic testing for hepatitis A and B, which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 4 of 50
4. Question
A 25-year-old woman comes to the office 1 week after she received an increased blood pressure reading at a health fair. She says that she also has had episodes of cramping of her legs and occasional headaches during the past 9 months. She takes no medications. Pulse is 80/min, and blood pressure is 160/98 mm Hg in the left upper extremity and 162/100 mm Hg in the right upper extremity. A bruit is heard over the left side of the abdomen. Cardiopulmonary examination shows no abnormalities. Ultrasonography of the kidneys with Doppler flow shows decreased blood flow to the left kidney. Which of the following sets of findings is most likely in this patient?
Option
Right Renal Vein Renin
Serum Aldosterone
Serum Potassium
A
↑
↑
↑
B
↑
↑
↓
C
↑
↓
↑
D
↑
↓
↓
E
↓
↑
↑
F
↓
↑
↓
G
↓
↓
↑
H
↓
↓
↓
CorrectIncorrect -
Question 5 of 50
5. Question
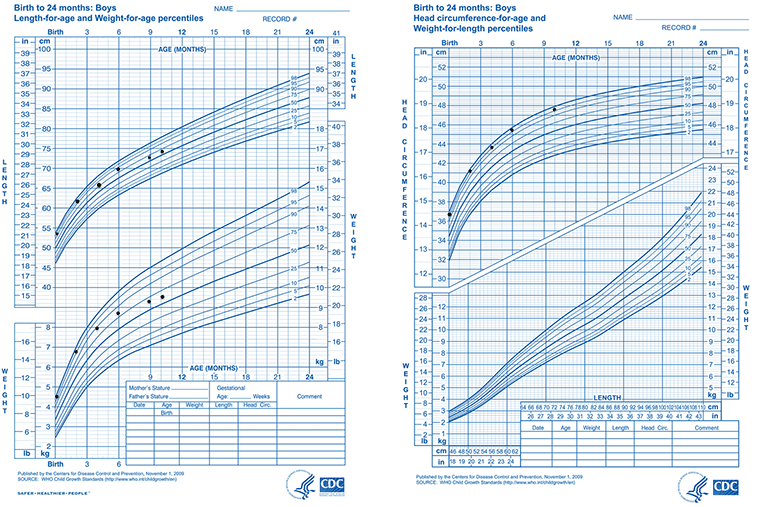
A 10-month-old boy is brought to the office by his parents for a well-child examination. His parents say they are concerned because people have told them his head seems too large for his body. He eats a variety of table foods and is able to feed himself soft foods with his hands. He drinks approximately 16 oz of breast milk by bottle daily and is breast-fed nightly. He crawls and takes steps holding onto his parents’ hands. He babbles and laughs. Medical history is unremarkable and he receives no medications. The patient’s growth charts are shown. Vital signs are within normal limits. Physical examination discloses no abnormalities. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 6 of 50
6. Question
A 60-year-old woman comes to the ambulatory surgical center to undergo a cardiac ablation. She has a history of six episodes of paroxysmal atrial fibrillation in the past 4 years. She has had four prior successful electrical cardioversions and spontaneously converted twice. Her only medication is rivaroxaban daily, which was prescribed 1 month ago. She is 160 cm (5 ft 3 in) tall and weighs 46 kg (101 lb); BMI is 18 kg/m2. Temperature is 37.0°C (98.6°F), pulse is 72/min and regular, respirations are 14/min, and blood pressure is 110/75 mm Hg. Physical examination shows no abnormalities. It is most appropriate for this patient to undergo a transesophageal echocardiography prior to the ablation procedure for the detection of which of the following?
CorrectIncorrect -
Question 7 of 50
7. Question
A 54-year-old man comes to the office for a routine health maintenance examination. Medical history is remarkable for well-controlled hypertension. Medications are hydrochlorothiazide and lisinopril. The patient’s wife died of breast cancer 2 years ago. During the past 9 months, he has had unprotected sexual intercourse with three female partners. Temperature is 37.6°C (99.7°F), pulse is 70/min, respirations are 16/min, and blood pressure is 128/70 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 100%. Physical examination shows no abnormalities. HIV antibody/antigen testing is positive. CD4+ T-lymphocyte count is 800/mm3. Results of testing for hepatitis B, hepatitis C, and syphilis are negative. A PPD skin test shows 7 mm of induration at 48 hours. Chest x-ray shows no abnormalities. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 8 of 50
8. Question
A 1-month-old boy is brought to the physician by his 17-year-old mother for a well-child examination. He is at the 30th percentile for length and 25th percentile for weight. During the examination, his mother reports that she is feeling stressed by the demands of motherhood. She and her son are living with her parents, and she does not get along well with them. She also notes that she is becoming increasingly irritable with her son whom she frequently finds difficult to soothe. She is breast-feeding but finds the process difficult and frustrating. She says that she is not depressed but has feelings of sadness and inadequacy. She still takes pleasure in activities she typically enjoys. She has not had suicidal ideation. Her sleep is disrupted by her newborn at night, but she is learning to nap when her baby sleeps. Observation of the mother-newborn dyad shows difficulty with reading the newborn’s cues. The mother appears distracted during an attempt to feed her son. Which of the following is the most appropriate recommendation?
CorrectIncorrect -
Question 9 of 50
9. Question
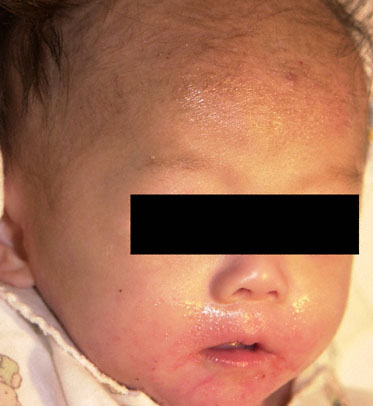
A 10-month-old girl is brought to the physician because of a 5-day history of a rash over the cheeks and diaper area that she constantly rubs. Her mother says that for the past 24 hours, her daughter has been unwilling to stand. She is afebrile and otherwise healthy. Her mother and 6-year-old brother have asthma. A photograph of the face is shown; a similar rash is noted over the diaper area. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 10 of 50
10. Question
A 72-year-old woman calls the clinic because of a 3-day history of frequent urination, urinary urgency, and pain with urination. She is currently visiting her daughter in a different state and has limited access to health care; she requests a prescription for antibiotics for a bladder infection be sent to a local pharmacy. The patient says that the only treatment that has improved her symptoms in the past is nitrofurantoin macrocrystals taken every 6 hours. The clinic nurse enters a prescription in the patient’s electronic health record (EHR) for the physician to sign; the prescription includes the correct medication but incorrect dosing instructions. The physician does not notice the error and signs the prescription to be sent to the pharmacy. When the physician is notified of the error by the pharmacist, the physician realizes that the nurse had chosen dosing for a similar antibiotic, nitrofurantoin monohydrate/macrocrystals, which is dosed twice daily. Which of the following interventions is most likely to prevent this error from recurring?
CorrectIncorrect -
Question 11 of 50
11. Question
The following vignette applies to the next 2 items. The items in the set must be answered in sequential order. Once you click Proceed to Next Item, you will not be able to add or change an answer.
A 23-year-old man with sickle cell disease is admitted to the hospital because of a 5-day history of shortness of breath and severe pain in his chest and legs. He has not had fever or cough. During the past 3 years, he has been hospitalized for painful sickle cell crises approximately twice yearly. Ten years ago, he underwent cholecystectomy for cholecystitis. His medications are folic acid and acetaminophen with codeine; 3 days ago, he began taking double his usual dose of acetaminophen with codeine to manage his increased pain. He does not smoke cigarettes, drink alcohol, or use illicit drugs. His temperature is 39°C (102.2°F), pulse is 120/min, respirations are 22/min, and blood pressure is 116/70 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 94%. The chest wall is tender to palpation. Bilateral basilar crackles are heard. His hemoglobin concentration is 9 g/dL, hematocrit is 27%, and leukocyte count is 15,000/mm3.
Item 1 of 2
Which of the following is the most appropriate next step in diagnosis?CorrectIncorrect -
Question 12 of 50
12. Question
The following vignette applies to the next 2 items. The items in the set must be answered in sequential order. Once you click Proceed to Next Item, you will not be able to add or change an answer.
Item 2 of 2
A chest x-ray shows small bilateral basilar infiltrates. Treatment with supplemental oxygen, intravenous antibiotics, and intravenous fluids is begun. Three days later, the patient’s shortness of breath is more severe. Pulse oximetry on 4 L/min of oxygen via nasal cannula shows an oxygen saturation of 94%. A chest x-ray shows increased infiltrates. Which of the following is the most appropriate next step in management?CorrectIncorrect -
Question 13 of 50
13. Question
A 17-year-old patient, gravida 1, para 0, aborta 1, is brought to the emergency department because of progressive vaginal bleeding and severe low abdominal pain since pregnancy ended in spontaneous abortion at 14 weeks’ gestation at home 2 hours ago. Pregnancy previously had been uncomplicated. She has hypothyroidism and takes levothyroxine and a prenatal vitamin. Temperature is 37.0°C (98.6°F), pulse is 100/min, respirations are 14/min, and blood pressure is 90/50 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 96%. She appears to be in mild distress. Pelvic examination shows a dilated cervix and active bleeding from the cervical os. Intravenous administration of fluids and morphine is begun, and laboratory studies are ordered. In addition to pelvic ultrasonography, which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 14 of 50
14. Question
Patient Information
Age: 68 years
Gender: M, self-identified
Race/Ethnicity: unspecified
Site of Care: intensive care unit (ICU)
History
Reason for Visit/Chief Concern: “I’ve been vomiting blood.”
History of Present Illness:
• 8-hour history of abdominal discomfort, with six episodes of bright red emesis and two episodes of melena
• reports weakness and light-headedness
Past Medical History:
• hypertension
• hypercholesterolemia
• gastroesophageal reflux disease
Medications:
• none
Allergies:
• no known drug allergies
Psychosocial History:
• drinks six beers weekly
• does not smoke cigarettes or use other substances
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
37.0°C
105/min
16/min
92/36 mm Hg
99%
178 cm
82 kg
26 kg/m2
(98.6°F)
on RA
(5 ft 10 in)
(180 lb)
• Appearance: fatigued; pale; awake and alert
• Skin: pale; cool to touch; dry
• HEENT: PERRL; no active bleeding from nares
• Pulmonary: clear; no wheezing
• Cardiac: tachycardic; no murmurs, rubs, or gallops
• Abdominal: hyperactive bowel sounds; soft; nondistended; no masses noted
• Extremities: no clubbing, cyanosis, or edema
• Neurologic: responds appropriately to questions; no focal deficits
Diagnostic Studies
Serum
Na+
142 mEq/L
K+
4.0 mEq/L
Cl–
104 mEq/L
HCO3–
26 mEq/L
Urea nitrogen
14 mg/dL
Creatinine
0.8 mg/dL
Glucose, nonfasting
129 mg/dL
Blood
Hematocrit
20.3%
Hemoglobin
6.2 g/dL
WBC
10,800/mm3
Platelet count
307,000/mm3
Question: The physicians responsible for the patient’s care discuss the risks of transfusing the patient with packed red blood cells with him and his family. Following consent and administration of two units of packed RBCs, which of the following is the most likely complication of blood transfusion in this patient?
CorrectIncorrect -
Question 15 of 50
15. Question
A 24-year-old nulligravid woman comes to the office because of a 6-month history of urinary urgency and moderate pain with urination and sexual intercourse. She has been avoiding intercourse with her partner during this time because of the pain. She has major depressive disorder and irritable bowel syndrome. Her only medication is bupropion. The patient has had no recent changes to her diet or bowel movements, except for occasional loose stools. She does not smoke cigarettes or drink alcoholic beverages. She is 174 cm (5 ft 7 in) tall and weighs 66 kg (145 lb); BMI is 23 kg/m2. Pulse is 82/min, and blood pressure is 127/85 mm Hg. The abdomen is soft and nontender. Bladder palpation reproduces discomfort similar to her pain. There is no cervical motion tenderness or discharge. Urine β-hCG testing, urine culture, and sexually transmitted infection screening are negative. Cystoscopy shows punctate hemorrhages in the bladder mucosa. The patient has temporary pain relief after saline distention of the bladder. Biopsy specimen of the bladder shows granulation across the mucosa, lamina propria, and muscularis layers and prominent mast cells. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 16 of 50
16. Question
A 76-year-old man is admitted to the hospital for management of severe dehydration. He says he is “fine” and has not felt like drinking much water lately. He was hospitalized 3 months ago following a cerebral infarction, which resulted in left-sided weakness. At that time, he was discharged to the care of his daughter. At discharge, he weighed 84 kg (186 lb). He has hyperlipidemia, hypertension, and benign prostatic hyperplasia. His medications are atorvastatin, enalapril, finasteride, and aspirin. On questioning, he says his daughter is away most of the time and sometimes forgets to buy groceries. He last saw her 3 days ago. He says he would like to live with his son. Today, the patient is 178 cm (5 ft 10 in) tall and weighs 73 kg (162 lb); BMI is 23 kg/m2. Pulse is 80/min, and blood pressure is 100/66 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 94%. Examination shows decreased skin turgor. Muscle strength is 3/5 in the left extremities. On mental status examination, he describes his mood as “fine” and has a distant affect. There is no evidence of suicidal ideation. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 17 of 50
17. Question
A 32-year-old woman, gravida 2, para 2, comes to the office for a routine health maintenance examination. She feels well. She has no history of serious illness. Her only medication is a contraceptive ring, which she started 6 weeks ago. Her mother received the diagnosis of breast cancer 1 week ago at the age of 68 years, and her paternal aunt died of breast cancer at the age of 61 years. The patient does not smoke cigarettes. She is 168 cm (5 ft 6 in) tall and weighs 87 kg (191 lb); BMI is 31 kg/m2. Blood pressure is 150/90 mm Hg. Examination shows no other abnormalities. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 18 of 50
18. Question
A 65-year-old woman comes to the office because of a 3-month history of mild abdominal discomfort and bloating. She has not had vaginal bleeding. Medical history is unremarkable, and she does not use any medications or other substances. She is 165 cm (5 ft 4 in) tall and weighs 82 kg (181 lb); BMI is 30 kg/m2. Vital signs are within normal limits. Physical examination discloses no abnormalities. Pelvic examination discloses a large right adnexal mass. Ultrasonography confirms the presence of a complex solid and cystic mass. Oophorectomy is done; resection results show a 10-cm cystic ovary with solid papillary excrescences composed of a highly atypical cellular proliferation with fibrovascular cores and epithelial tufting. There are also numerous nodules measuring up to 1 cm in diameter on the omentum. Recurrence of disease in this patient should be monitored periodically with which of the following serum concentration studies?
CorrectIncorrect -
Question 19 of 50
19. Question
A 57-year-old woman comes to the physician because of a 1-week history of decreased vision in her right eye. Four months ago, she began topiramate therapy for seizure disorder. She has no other history of serious illness and takes no other medications. Examination of the right eye shows an injected conjunctiva and a steamy cornea. Dilated funduscopic examination is limited and shows a good red reflex. The left pupil is 4 mm and reactive to light; the right pupil is 4 mm and nonreactive to light. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 20 of 50
20. Question
Patient Information
Age: 78 years
Gender: F, self-identified
Race/Ethnicity: unspecified
Site of Care: acute rehabilitation facility
History
Reason for Admission/Chief Concern: day 5 of admission following surgical nailing of intertrochanteric fracture
History of Present Illness:
• sustained left intertrochanteric fracture in motor vehicle collision 10 days ago
• underwent uncomplicated emergent left intramedullary nailing of the fracture
• began physical therapy immediately after the procedure and has progressed well
• admitted to the acute rehabilitation facility for strengthening and gait training
• 5-day history of nausea, since admission to the facility
• patient reports that she still “feels weak”
Past Medical History:
• hypertension
• type 2 diabetes mellitus
• gastroesophageal reflux disease
Medications:
• metformin
home, continued in hospital and rehabilitation facility
• lisinopril
home, continued in hospital and rehabilitation facility
• amlodipine
initiated on admission to rehabilitation facility
• metoclopramide, prn for nausea
initiated on admission to rehabilitation facility
• promethazine, prn for nausea
initiated on admission to rehabilitation facility
• acetaminophen, prn for pain
initiated on admission to rehabilitation facility
• furosemide, prn for edema
initiated on rehabilitation facility day 4
Allergies:
• no known drug allergies
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
36.7°C
72/min
15/min
100/70 mm Hg
93%
173 cm
82 kg
27 kg/m2
(98.0°F)
on RA
(5 ft 8 in)
(180 lb)
• Appearance: uncomfortable; no acute distress
• Pulmonary: unlabored breathing; clear to auscultation
• Cardiac: regular rhythm; no murmurs
• Abdominal: normoactive bowel sounds; soft, nontender to palpation
• Extremities: grade 1+ bilateral lower extremity edema; no cyanosis
• Neurologic: resting tremors on both distal upper extremities at a rate of 6 Hz
Diagnostic Studies
Serum
Na+
135 mEq/L
K+
4.8 mEq/L
Cl−
94 mEq/L
HCO3−
24 mEq/L
Urea nitrogen
12 mg/dL
Creatinine
1.0 mg/dL
Glucose, nonfasting
130 mg/dL
Calcium
10.0 mg/dL
Blood
Hematocrit
37%
Hemoglobin
12.5 g/dL
WBC
5500/mm3
Neutrophils, segmented
64%
Lymphocytes
36%
Platelet count
300,000/mm3
Hemoglobin A1c
7.2%
Question: Which of the following is the most likely complication of this patient’s current condition?
CorrectIncorrect -
Question 21 of 50
21. Question
A 3-year-old boy is brought to the office by his father because of a 2-month history of intermittently bloody stools. The father describes the stools as hard balls and says that there are often streaks of blood on the outside. The patient has a bowel movement every 1 to 2 days. He is fully toilet trained for urine but refuses to use the toilet to stool. During the past week, his appetite has decreased, and he has only been picking at foods. He eats the same meals as his family but does not like most vegetables. The only fruits he eats are bananas and grapes. He drinks 24 to 28 oz of low-fat cow milk daily. His father reports no changes to his urination. Medical history is unremarkable and he receives no medications. Vaccinations are up-to-date. He is 90 cm (2 ft 11 in; 10th percentile) tall and weighs 12.5 kg (27.5 lb; 10th percentile); BMI is 15.4 kg/m2 (30th percentile). Temperature is 37.6°C (99.7°F), pulse is 120/min, respirations are 22/min, and blood pressure is 90/64 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 98%. Bowel sounds are normoactive. There is diffuse mild tenderness to palpation of the abdomen with no rebound tenderness or guarding. The remainder of the physical examination discloses no abnormalities. Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 22 of 50
22. Question
A 47-year-old woman comes to the office because of a 3-day history of fever, fatigue, and loss of appetite. Five weeks ago, she underwent uncomplicated kidney transplant for end-stage kidney disease caused by type 2 diabetes mellitus. Her postoperative course had been uncomplicated and stable with her current immunosuppression therapy. Medical history is also remarkable for hypercholesterolemia and essential hypertension. Medications are insulin, prednisone, cyclosporine, mycophenolate mofetil, atorvastatin, and irbesartan. Temperature is 38.0°C (100.4°F), pulse is 100/min, respirations are 16/min, and blood pressure is 146/90 mm Hg. Abdominal examination shows a well-healing incision and tenderness to palpation over the right lower quadrant at the transplant site. There is 1+ pedal edema. Results of laboratory studies are shown:
Leukocyte count
4500/mm3
Serum
Na+
130 mEq/L
K+
5.5 mEq/L
Cl−
92 mEq/L
HCO3−
20 mEq/L
Urea nitrogen
34 mg/dL
Creatinine
3.1 mg/dL
Glucose
180 mg/dL
Which of the following is the most likely explanation for these findings?
CorrectIncorrect -
Question 23 of 50
23. Question
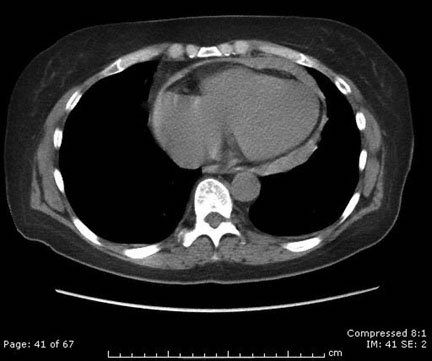
A 27-year-old man comes to the office because of a 2-day history of moderate chest pain and shortness of breath. He also has a 1-week history of a cough and low-grade fever that have not improved. He has no personal or family history of major medical illness. Temperature is 38.0°C (100.4°F), pulse is 92/min, respirations are 20/min, and blood pressure is 95/65 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 97%. The lungs are clear to auscultation. Distant heart sounds are heard, and an anterior friction rub is heard and palpated. Results of laboratory studies, including complete blood count, and serum concentrations of electrolytes, urea nitrogen, and creatinine, are within the reference ranges. CT scan of the chest is shown. Which of the following is the most likely cause of these findings?
CorrectIncorrect -
Question 24 of 50
24. Question
A 12-year-old boy is brought to the physician for a routine examination. He has a history of aortic root enlargement, mitral valve prolapse, and lens dislocation that was surgically repaired at 2 years of age. His father and one of his three siblings have similar histories and physical findings. He is at the 95th percentile for height and 25th percentile for weight. Examination shows long fingers and toes, hyperextensible joints, pectus excavatum, and scoliosis. Which of the following best describes the mode of inheritance of this patient’s condition?
CorrectIncorrect -
Question 25 of 50
25. Question
A 19-year-old man comes to the emergency department because of a 3-hour history of severe chest pain below the sternum. The pain is described as sharp and pleuritic and radiates to his back. He also reports pain with swallowing and shortness of breath. He says he “drank a lot of alcohol” at a party yesterday evening and had several episodes of nonbloody vomiting this morning; his current symptoms began 1 hour later. He has gastroesophageal reflux disease and generalized anxiety disorder. Medications are omeprazole and escitalopram. The patient has no known allergies. He drinks alcoholic beverages “heavily” on weekends; he does not smoke cigarettes or use any other substances. He is 178 cm (5 ft 10 in) tall and weighs 77 kg (170 lb); BMI is 24 kg/m2. Temperature is 37.6°C (99.6°F), pulse is 138/min, respirations are 20/min, and blood pressure is 87/40 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 95%. The patient appears confused but is in no respiratory distress. Pulmonary examination discloses tachypnea with shallow inspirations. Cardiac examination discloses tachycardia and normal S1 and S2. There is tenderness to palpation of the anterior chest wall. Bowel sounds are normal. Abdomen is diffusely tender to palpation. The remainder of the physical examination discloses no abnormalities. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 26 of 50
26. Question
A 25-year-old woman comes to the office because of a 1-month history of a lump in her neck. The lump has remained unchanged in size during this time. She has not had pain, difficulty swallowing, or difficulty breathing. Medical history is remarkable for generalized anxiety disorder diagnosed 5 years ago. Her only medication is an oral contraceptive. She had been receiving care from a mental health counselor for 3 years but discontinued seeing the counselor 3 months ago because of financial difficulties. Family history is remarkable for papillary thyroid cancer in the patient’s mother. The patient is 173 cm (5 ft 8 in) tall and weighs 57 kg (125 lb); BMI is 19 kg/m2. Temperature is 37.1°C (98.7°F), pulse is 88/min, respirations are 17/min, and blood pressure is 101/72 mm Hg. Palpation of the neck discloses a firm, 2-cm nodule in the right lobe of the thyroid gland. There is a mild tremor in both hands. Results of laboratory studies show a serum TSH concentration of 3.5 µU/mL and free T4 concentration of 1.2 ng/dL. Ultrasonography of the thyroid gland shows a 2-cm hypoechoic nodule in the right inferior lobe. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 27 of 50
27. Question

A 5-minute-old boy is admitted to the neonatal intensive care unit because of absent breath sounds on the left, significant respiratory distress with increased work of breathing, and profound hypoxia that developed 5 minutes after birth. The patient was born at 36 weeks’ gestation to a 21-year-old primigravid woman via normal spontaneous vaginal delivery. The pregnancy was uncomplicated despite no prenatal care. The newborn’s temperature is 37.2°C (99.0°F), pulse is 170/min, and respirations are 40/min. Pulse oximetry on room air shows an oxygen saturation of 82%. The patient is intubated. Physical examination discloses fair breath sounds on the right and absent breath sounds on the left. Bowel sounds are auscultated in the left hemithorax. The remainder of the physical examination, including abdominal examination, discloses no abnormalities. Chest x-ray is shown. Which of the following anatomic abnormalities is most likely to be found in this patient?
CorrectIncorrect -
Question 28 of 50
28. Question
An 80-year-old man comes to the office for a routine examination. He says he fell in the grocery store last week but feels well overall. He did not have light-headedness, palpitations, or chest pain before the fall, and he did not hit his head or have loss of consciousness. He has no history of other falls during the past year. He sustained a pulmonary embolism 2 months ago. He has hypertension, stage 2 chronic kidney disease, and osteoarthritis. Medications are amlodipine, lisinopril, dabigatran, and acetaminophen. Temperature is 37.6°C (99.7°F), pulse is 70/min, respirations are 16/min, and blood pressure is 140/80 mm Hg while sitting. Within 2 minutes after standing, pulse is 70/min, and blood pressure is 135/80 mm Hg. He appears well. Examination shows a large ecchymosis on the right upper extremity. Cardiopulmonary examination discloses no abnormalities. He performs a Timed Up and Go test in 30 seconds, indicating he is at increased fall risk. Which of the following is the most appropriate recommendation at this time?
CorrectIncorrect -
Question 29 of 50
29. Question
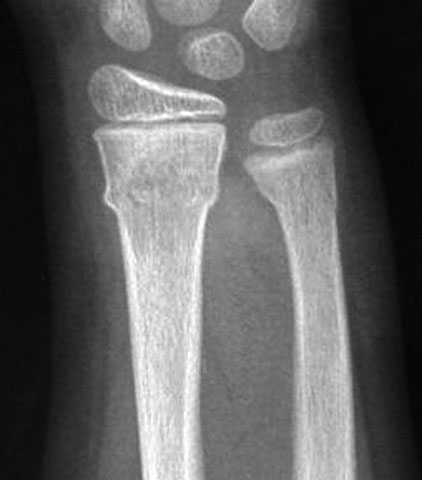
A 15-year-old girl is brought to the emergency department 1 hour after she fell onto her outstretched right arm while playing soccer. She experienced immediate pain. She says she did not think the injury was serious and was able to finish the game. She has not had weakness, numbness, or any other symptoms in her right hand and wrist. On arrival, she is in no distress. Her pulse is 60/min, respirations are 12/min, and blood pressure is 110/60 mm Hg. Examination of the right upper extremity shows moderate tenderness over the distal radius. There is no swelling, erythema, or deformity. Capillary refill time in the fingers of the right hand is 2 seconds. An x-ray of the right wrist is shown. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 30 of 50
30. Question
A 35-year-old woman comes to the clinic because of a 4-month history of progressive fatigue when running or walking long distances. She also has had occasional episodes of mild shortness of breath and light-headedness that resolve with rest. Medical history is remarkable for hypertension and type 2 diabetes mellitus that both resolved 3 years ago after she underwent Roux-en-Y gastric bypass. Since the procedure, she has lost 45 kg (100 lb). Her only medication is a multivitamin with iron, calcium, and vitamin D. She drinks three to four glasses of wine weekly; she does not smoke cigarettes or use other substances. She exercises by walking, running, or doing yoga five times weekly. She is 165 cm (5 ft 5 in) tall and weighs 70 kg (155 lb); BMI is 26 kg/m2. Temperature is 36.5°C (97.7°F), pulse is 98/min, respirations are 14/min, and blood pressure is 110/60 mm Hg. Examination shows no abnormalities except for pale conjunctivae. Results of laboratory studies are shown:
Hematocrit
24%
Hemoglobin
8.0 g/dL
MCV
105 μm3
WBC
4500/mm3
Platelet count
155,000/mm3
Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 31 of 50
31. Question
Patient Information
Age: 17 years
Gender: F, self-identified
Race/Ethnicity: unspecified
Site of Care: clinic
History
Reason for Visit/Chief Concern: “I am having trouble sleeping.”
History of Present Illness:
• 2-month history of waking up early in the morning with difficulty falling back to sleep
• over-the-counter melatonin has not helped her sleep
• feels tired all day and sad most of the time
• has no interest in doing things she used to enjoy, such as playing basketball or spending time with her friends
• has been skipping school frequently to stay at home
• worries about what she will do after high school and feels “alone”
• does not feel close with her parents and does not tell them much about what is going on in her life
• feels like she is always eating but is never really hungry; has had a 2.3-kg (5-lb) weight gain since the start of school 3 months ago
Past Medical History:
• mild intermittent asthma well controlled with albuterol
Medications:
• inhaled albuterol prn for difficulty breathing
• melatonin prn for difficulty sleeping
Vaccinations:
• up-to-date
Allergies:
• no known drug allergies
Family History:
• unknown; adopted as an infant and does not know her biological parents
Psychosocial History:
• lives at home with adoptive parents
• currently in the 12th grade
• attracted to males and had a boyfriend that she broke up with 6 months ago; has never been sexually active
• tried alcoholic beverages and cannabis in the past but does not like how they make her feel, so she does not use them regularly
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
37.0°C
80/min
12/min
110/60 mm Hg
98%
174 cm
80 kg
26.4 kg/m2
(98.6°F)
on RA
(5 ft 9 in)
(176 lb)
89th %ile
95th %ile
95th %ile
• Appearance: quiet, tearful at times; responds briefly to all questions
• Skin: warm and well perfused; no rash; capillary refill time <2 seconds
• HEENT: moist mucous membranes, clear oropharynx
• Pulmonary: clear to auscultation; no wheezes
• Cardiac: regular rhythm; no murmurs
• Abdominal: nondistended; normoactive bowel sounds; soft, nontender
• Neurologic: alert; no focal motor or sensory deficits
• Psychiatric: depressed mood; no active suicidal ideation but says she thinks that “everything would be better if I were not here”
Question: Which of the following is the most appropriate pharmacotherapy at this time?
CorrectIncorrect -
Question 32 of 50
32. Question
The director of a cardiac surgery group at an urban medical center would like to improve its performance related to the control of postoperative blood glucose concentrations. The director reviewed relevant publications from the past 10 years and found that patients who have blood glucose concentrations of less than 150 mg/dL have a decreased risk of infection postoperatively. The director subsequently implements a protocol for perioperative patients that includes hourly blood glucose testing with concomitant titrated intravenous insulin dosing. Two months after this intervention is implemented, the director measures the incidence of hypoglycemia in patients who have undergone cardiac surgery at the medical center. Which of the following best describes this assessment?
CorrectIncorrect -
Question 33 of 50
33. Question
A 50-year-old man comes to the office to request the herpes zoster vaccine. He has mild, persistent asthma well controlled with daily inhaled fluticasone therapy during the past 5 years. He says that he has episodes of wheezing, chest tightness, and cough one to two times weekly; these symptoms awaken him at night once or twice monthly. He has no other history of major medical illness and takes no other medications. Vital signs are within normal limits. Physical examination shows no abnormalities. Prior to administration of the herpes zoster vaccine, the most appropriate next step in treatment is to switch fluticasone to which of the following drugs?
CorrectIncorrect -
Question 34 of 50
34. Question
A 21-year-old woman comes to the clinic because of a 3-week history of progressive fatigue, increased thirst, and increased urinary frequency. She feels thirsty despite drinking more water than usual. Her appetite also has increased during this time, but she thinks she may have lost some weight. She has no history of serious illness or operative procedures and takes no medications. She does not smoke cigarettes or drink alcoholic beverages. She is 163 cm (5 ft 4 in) tall and weighs 50 kg (111 lb), which is a 4.5-kg (10-lb) weight loss since her last examination; BMI is 19 kg/m2. Temperature is 37.0°C (98.6°F), pulse is 110/min, respirations are 20/min, and blood pressure is 110/70 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 98%. Physical examination discloses no abnormalities. Results of which of the following laboratory studies are most likely to be abnormal in this patient?
CorrectIncorrect -
Question 35 of 50
35. Question
A 32-year-old woman comes to the office because of a 1-day history of severe back pain that radiates down her legs, dragging of her right leg, and difficulty emptying her bladder. She also has a 3-day history of tingling and numbness that began in her feet and progressed up her calves and thighs to her waist. She has not had fever, headache, vision changes, or changes in muscle strength in her arms. One week ago, she had an upper respiratory tract infection with nonproductive cough. She takes no medications. Temperature is 37.0°C (98.6°F), pulse is 84/min, respirations are 18/min, and blood pressure is 132/78 mm Hg. She appears anxious but not in distress. Physical examination discloses mild lower abdominal tenderness and midline fullness. Deep tendon reflexes are absent in the lower extremities. Sensation to pinprick is decreased below the umbilicus. Placement of a urinary catheter drains 1 L of clear urine. MRI of the spine is most likely to show which of the following findings in this patient?
CorrectIncorrect -
Question 36 of 50
36. Question
A 22-year-old woman is brought to the emergency department by her boyfriend 30 minutes after he found her unresponsive in the bathroom. He last saw her 20 minutes prior to this, and she had appeared healthy. He says that she has no known history of major medical illness, but that she has used heroin in the past. Her temperature is 37.0°C (98.6°F), pulse is 80/min, and blood pressure is 98/60 mm Hg. She is obtunded and only responds to painful stimuli. Which of the following sets of findings is most likely in this patient at this time?
Option
Respirations (/min)
PCO₂ (mm Hg)
PO₂ (mm Hg)
A
6
80
45
B
10
40
65
C
12
60
80
D
16
80
65
E
20
20
65
CorrectIncorrect -
Question 37 of 50
37. Question
A 27-year-old primigravid woman at 24 weeks’ gestation is brought to the emergency department because of a 2-hour history of contractions every 3 minutes that last 60 seconds. Her pregnancy had been uncomplicated. She has no history of serious illness or operative procedures. The cervix is 4 cm dilated and 75% effaced; the vertex is at –1 station. The membranes are intact. The remainder of the examination shows no abnormalities. The patient asks what can be done to halt preterm labor. The physician reviews a recent randomized trial in which 10% of women in preterm labor who receive a tocolytic agent deliver within 48 hours versus 14% of those in a placebo group (p=0.23). Based on these data, which of the following best describes this patient’s risk for delivering within 48 hours of tocolysis relative to expectant management?
CorrectIncorrect -
Question 38 of 50
38. Question
Patient Information
Age: 10 years
Gender: M, self-identified
Race/Ethnicity: African American, self-identified
Site of Care: office
History
Reason for Visit/Chief Concern: “My left knee hurts.”
History of Present Illness:
• 1-month history of daily left knee pain that has worsened during the past week
• pain is worse later in the day or with activity
• rates pain as a 4 on a 10-point scale; worse with running
• plays soccer and has to occasionally sit out of practice and games because of pain
• application of ice to the knee after playing soccer provides moderate relief
• no known trauma or knee injuries
• no difficulty sleeping
Past Medical History:
• no serious illnesses
Medications:
• ibuprofen prn for pain
Vaccinations:
• up-to-date
Allergies:
• no known drug allergies
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
37.0°C
86/min
16/min
116/72 mm Hg
100%
139 cm
32 kg
16.6 kg/m2
(98.6°F)
on RA
(4 ft 7 in)
(71 lb)
48th %ile
50th %ile
50th %ile
• Appearance: alert, cooperative, comfortable
• Extremities: no warmth, edema, effusion, or tenderness of the left knee joint; point tenderness of the left tibial tuberosity; left tibial tuberosity appears larger than right; full range of motion of the left lower extremity; examination of the right knee discloses no abnormalities
Question: Which of the following is the most likely diagnosis?
CorrectIncorrect -
Question 39 of 50
39. Question
A previously healthy 52-year-old man is brought to the emergency department because of right lower leg pain that began this morning and has become increasingly severe with walking. He has smoked one pack of cigarettes daily for 30 years and drinks two to three beers daily. Vital signs are within normal limits. Examination of the right leg shows calf tenderness. There is no pedal edema. Serum D-dimer concentration is increased. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 40 of 50
40. Question
A 16-year-old girl is brought to the clinic because of a 6-month history of worsening anxiety and depressed mood. During this time, she also has had insomnia and occasional thoughts of not wanting to live anymore because “I’m just so tired of worrying about everything all of the time; it’s like my brain doesn’t get a break.” She reports constant worry about her academic performance and safety of family members. She has generalized anxiety disorder and sees a therapist weekly. The patient takes no prescription medications. Vital signs are within normal limits. Physical examination discloses no abnormalities. The patient states that she has had suicidal thoughts but has no current plan to harm herself or others. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 41 of 50
41. Question
Patient Information
Age: 21 years
Gender: F, self-identified
Race/Ethnicity: White, self-identified
Site of Care: office
History
Reason for Visit/Chief Concern: “I had blurry vision and now I have a headache.”History of Present Illness:
• developed blurred vision in right eye 2 hours ago while taking an examination for graduate school class
• blurriness began in center of visual field and gradually expanded
• blurred vision resolved spontaneously after 20 minutes
• reports 90-minute history of left-sided headache
• describes headache as pounding
• felt nauseated by odor of classmate’s cologne
• managed to complete her examination before coming to office
• now asks to lie down in a dark room because she feels fatigued
Past Medical History:
• asthma
• motion sickness
Medications:
• oral contraceptive
• albuterol (inhaled)
Allergies:
• penicillin (rash)
Family History:
• patient is adopted; family history unknown
Psychosocial History:
• drinks two alcoholic beverages weekly
• occasionally smokes cannabis
• does not smoke cigarettes
• reports increased stress since studying for examination during past 2 days
Physical Examination
Temp
Pulse
Resp
BP
O2 Sat
Ht
Wt
BMI
37.0°C
74/min
18/min
120/72 mm Hg
99%
152 cm
58 kg
25 kg/m2
(98.6°F)
on RA
(5 ft)
(128 lb)
• Appearance: lying supine on examination table
• Skin: no lesions, bruises, or discoloration
• HEENT: no papilledema; pupils reactive to light; visual fields are full to confrontation
• Neck: nontender to palpation; no meningismus
• Pulmonary: mild expiratory wheezes bilaterally
• Cardiac: regular rhythm; no murmurs, rubs, or gallops
• Abdominal: nontender to palpation; no organomegaly
• Neurologic: fully oriented; cranial nerves intact; muscle strength 5/5 in upper and lower extremities
Question: Which of the following is the most appropriate diagnostic study at this time?
CorrectIncorrect -
Question 42 of 50
42. Question
An 85-year-old woman, who has advanced breast cancer, is receiving home hospice care. Her son, who is her primary caregiver, calls her primary physician because she has a 4-hour history of confusion in addition to back pain, which has been increasingly severe during the past week. Medications are sublingual morphine, sublingual lorazepam, topical diclofenac, and bisacodyl suppositories; doses already have been administered for the day. The physician has been caring for this patient for 15 years and knows that she finds comfort in her spirituality, values her independence, has a low tolerance for pain, and has expressed a desire to receive her end-of-life care at home. The patient’s son says that his mother’s eyes are closed, and her eyebrows are furrowed. She continuously attempts to shift her position in bed and is muttering incomprehensibly. Which of the following is the most appropriate next step?
CorrectIncorrect -
Question 43 of 50
43. Question
A 23-year-old woman comes to the emergency department (ED) 4 days after her husband hit her in the left ear and face after he returned home intoxicated. She has had decreased hearing in the left ear since that time. She says the altercation ended with rough, nonconsensual intercourse. Her husband was not wearing a condom. The patient thought her injuries would heal without medical intervention, but she decided to seek treatment when her hearing did not improve. During the interview, she minimizes her injuries and makes excuses for her husband, saying that he is sorry for his actions and has promised to get treatment for his intravenous drug use. Review of the patient’s electronic medical record shows that she has had multiple visits to the ED for physical injuries. She has no other history of serious illness and takes no medications. She does not drink alcohol, smoke cigarettes, or use illicit drugs. The patient appears tearful and subdued. She is 163 cm (5 ft 4 in) tall and weighs 48 kg (105 lb); BMI is 18 kg/m2. Temperature is 37.0°C (98.6°F), pulse is 80/min, respirations are 16/min, and blood pressure is 100/70 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 98%. Physical examination shows partially healed ecchymoses over the left zygomatic arch and forearms. The left tympanic membrane is perforated. Anogenital examination shows lacerations around the anus. Urine pregnancy test result is positive. Which of the following factors would most strongly influence the physician’s decision not to provide this patient with HIV postexposure prophylaxis?
CorrectIncorrect -
Question 44 of 50
44. Question
An 18-year-old woman comes to the emergency department 1 hour after the sudden onset of worsening “waves” of lower abdominal pain, followed by nausea and vomiting. Her symptoms are not affected by body positioning. She has no history of serious illness or operative procedures. She takes no medications. Temperature is 37.0°C (98.6°F), pulse is 125/min, respirations are 25/min, and blood pressure is 135/90 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 100%. Palpation of the abdomen discloses diffuse tenderness with rebound tenderness. Pelvic examination discloses right adnexal fullness and no cervical motion tenderness. Urine pregnancy test result is negative. Pelvic ultrasonography discloses an 8-cm simple cystic right ovarian mass with indeterminate Doppler flow. Which of the following is the most appropriate surgical management of the patient’s right ovary and fallopian tube?
CorrectIncorrect -
Question 45 of 50
45. Question
A 16-year-old girl is brought to the office by her mother because of a 2-day history of nausea, vomiting, and loss of appetite. The patient says that 3 days ago, she ingested half a bottle of her mother’s acetaminophen after her boyfriend broke up with her. She has no history of major medical illness. Her only medication is an oral contraceptive. She appears ill. Her temperature is 37.2°C (99.0°F), pulse is 98/min, respirations are 18/min, and blood pressure is 110/72 mm Hg. Physical examination shows moderate conjunctival icterus, and diffuse jaundice and abdominal tenderness. Examination of a liver biopsy specimen is most likely to show which of the following abnormalities?
CorrectIncorrect -
Question 46 of 50
46. Question
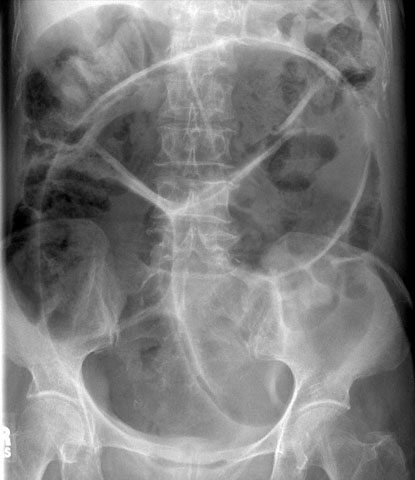
An 82-year-old man with dementia, Alzheimer type, is transferred from a skilled nursing care facility to the hospital because of a progressive abdominal distention for 2 days. During this time, he has not had a bowel movement. He has a history of hypertension. Current medications include a β-adrenergic blocking agent, diuretic, and serotonin agonist. Abdominal examination shows distention without tenderness, rigidity, or guarding. The remainder of the examination shows no abnormalities. X-ray of the abdomen is shown. Which of the following is the most appropriate next step in management?
CorrectIncorrect -
Question 47 of 50
47. Question
A 23-year-old woman comes to the clinic because she believes she is pregnant. Her last menstrual period was 6 weeks ago, and a home urine pregnancy test result was positive. She has type 2 diabetes mellitus that was diagnosed at the age of 14 years. She takes daily insulin glargine and insulin lispro before meals. Her regimen has been unchanged during the past 2 years. Temperature is 37.0°C (98.6°F), pulse is 87/min, respirations are 13/min, and blood pressure is 116/79 mm Hg. Physical examination shows no abnormalities. Serum glucose concentration is 122 mg/dL and hemoglobin A1c is 8.2%. Urine β-hCG test result is positive. This patient’s fetus is at greatest risk for developing which of the following conditions?
CorrectIncorrect -
Question 48 of 50
48. Question
A 35-year-old woman comes to the office because of right knee pain that began suddenly yesterday. She rates her current pain as an 8 on a 10-point scale. She reports no other symptoms. Medical history is remarkable for an episode of bacterial meningitis at age 15 years that resolved with no complications. She takes no medications. She has no known drug allergies. She drinks one glass of wine with dinner 5 nights weekly and occasionally smokes cannabis. She does not smoke cigarettes. She is sexually active and uses condoms inconsistently. Her last menstrual period ended 2 days ago. She is 160 cm (5 ft 3 in) tall and weighs 61 kg (135 lb); BMI is 24 kg/m2. Temperature is 37.0°C (98.6°F), pulse is 74/min, respirations are 16/min, and blood pressure is 110/80 mm Hg. The patient appears well developed and well nourished. Skin examination shows no lesions. Lungs are clear to auscultation. Cardiac examination discloses a regular rhythm with no murmurs, rubs, or gallops. The right knee is moderately erythematous and edematous and is tender to palpation. Range of motion in the right knee is decreased. The remainder of the physical examination discloses no abnormalities. Results of laboratory studies are shown:
Blood
Hematocrit
35%
Hemoglobin
13.0 g/dL
WBC
7500/mm3
Platelet count
162,000/mm3
Synovial Fluid (3.5 mL from right knee)
Appearance
Yellow, opaque
WBCs
20,000/mm3
Neutrophils, segmented
75%
Results of synovial fluid cultures are pending. Which of the following infectious agents is the most likely cause of this patient’s condition?
CorrectIncorrect -
Question 49 of 50
49. Question
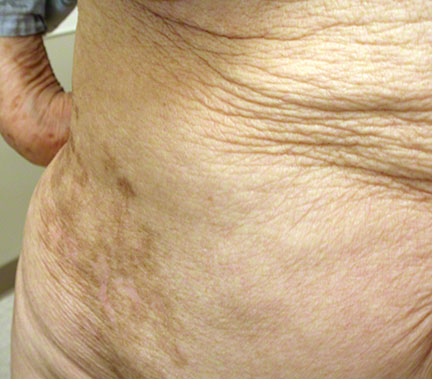
A 62-year-old woman comes to the office because of a 5-month history of persistent painful marks on the right side of her abdomen. She also says her appetite has been decreased since her last office visit 2 years ago. At that visit, the patient was evaluated for painful forehead lesions and was diagnosed with herpes zoster. Acyclovir therapy was prescribed, but the patient was lost to follow-up. Today, she says she took “most” of the acyclovir and that her forehead lesions resolved. Prior to that visit, she had not been evaluated by a physician for more than 15 years. Medical history also is remarkable for cocaine use for 5 years when she was in her 30s. She takes no routine medications. Vaccinations are not up-to-date. She does not smoke cigarettes, drink alcoholic beverages, or use any other substances. She has had multiple sexual partners since her last visit; she uses condoms inconsistently. She is unemployed and has not traveled outside of the United States recently. She is 165 cm (5 ft 5 in) tall and weighs 86 kg (190 lb); BMI is 32 kg/m2. Temperature is 37.1°C (98.7°F), pulse is 89/min, respirations are 18/min, and blood pressure is 130/80 mm Hg. Examination of the skin discloses the findings shown in the photograph. The rash is extremely tender to light touch. The remainder of the physical examination discloses no abnormalities. Which of the following is most likely to have prevented this patient’s condition?
CorrectIncorrect -
Question 50 of 50
50. Question
A previously healthy 27-year-old woman comes to the physician because of a 2-week history of intermittent, severe headaches. She has not had dizziness, vertigo, light sensitivity, nausea, or vomiting. She takes no medications. Her temperature is 37°C (98.6°F), pulse is 70/min, respirations are 18/min, and blood pressure is 190/100 mm Hg. Examination shows no jugular venous distention. No murmurs or gallops are heard on cardiac examination. A bruit is heard in the epigastrium. Serum studies show:
Na+
147 mEq/L
K+
3.0 mEq/L
Cl−
110 mEq/L
HCO3−
28 mEq/L
Creatinine
1.1 mg/dL
A CT scan of the head shows no abnormalities. An increase in which of the following is the most likely cause of this patient’s increased blood pressure?
CorrectIncorrect
